In Mexico, there has been an upward trend in mortality rates from colorectal cancer (CRC) over the past three decades. This tumor is ranked among the ten most prevalent causes of morbidity from malignancies in Mexico.
AimsTo determine the mortality trends by socioeconomic region and by state, and to establish the relative risk between both educational level and socioeconomic region with mortality from CRC within the time frame of 2000-2012.
Materials and methodsRecords of mortality associated with colorectal cancer were obtained. Rates of mortality by state and by socioeconomic region were calculated, along with the strength of association (obtained through the Poisson regression) between both socioeconomic region and educational level and the mortality from CRC.
ResultsA total of 45,487 individuals died from CRC in Mexico from 2000 to 2012. Age-adjusted mortality rates per 100,000 inhabitants increased from 3.9 to 4.8. Baja California, Baja California Sur, and Sonora had the highest mortality from CRC. Individuals with no school or incomplete elementary school had a higher risk of dying from this cancer (RR of 3.57, 95% CI: 3.46-3.68). Region 7 had the strongest association with mortality from CRC (Mexico City: RR was 2.84, 95% CI: 2.39-3.37 [2000] and 3.32, 95% CI: 2.89-3.82 [2012]).
ConclusionsIn Mexico, the age-adjusted mortality rates per 100,000 inhabitants that died from CRC increased from 3.9 to 4.8 in the study period, using the world population age distribution as the standard. Baja California, Baja California Sur, and Sonora had the highest mortality from CRC. Mexico City, which was socioeconomic region 7, had the strongest association with mortality from CRC.
En México ha habido una tendencia al alza en las tasas de mortalidad por cáncer colorrectal (CCR) en las últimas 3 décadas. Esta neoplasia está clasificada dentro de las 10 causas más frecuentes de morbilidad por neoplasias malignas en México.
ObjetivosDeterminar las tendencias de la mortalidad por CCR por región socioeconómica y por estado, así como establecer el riesgo relativo entre el nivel de educación y la región socioeconómica con la mortalidad por CCR en el periodo 2000-2012.
Materiales y métodosSe obtuvieron los registros de mortalidad por CCR. Se calcularon las tasas de mortalidad por estado y por región socioeconómica, así como la fuerza de asociación (mediante la regresión de Poisson) entre la región socioeconómica y el nivel de educación con la mortalidad por CCR.
ResultadosEn México, en los años 2000-2012, 45,487 personas murieron por CCR. Las tasas de mortalidad ajustadas por edad por cada 100,000 habitantes se incrementaron de 3.9 a 4.8. Baja California, Baja California Sur y Sonora tuvieron la mayor mortalidad por CCR. Los individuos sin escolaridad o con primaria incompleta tuvieron un mayor riesgo de morir por esta neoplasia (RR de 3.57, IC del 95%:3.46-3.68). La región 7 presentó la mayor fuerza de asociación con la mortalidad por CCR (Ciudad de México: RR: 2.84, IC del 95%: 2.39-3.37 [2000] y RR: 3.32, IC del 95%: 2.89-3.82 [2012]).
ConclusionesEn México, las tasas de mortalidad ajustadas por edad por cada 100,000 habitantes que murieron por CCR se incrementaron de 3.9 a 4.8 en el periodo de estudio, tomando como estándar la distribución de edades en la población mundial. Baja California, Baja California Sur y Sonora tuvieron la mayor mortalidad por CCR. La Ciudad de México como región socioeconómica 7 presentó la mayor fuerza de asociación con la mortalidad por CCR.
In 2012, colorectal cancer (CRC) was the third most common cancer in men worldwide, with 746,000 cases, representing 10% of all malignant tumors. It was the second most common cancer in women, with 614,000 cases, corresponding to 9.2% of all malignancies. According to the 2012 GLOBOCAN health project, almost 55% of cases of CRC occur in the more developed regions. There is a wide geographic variation in incidence of this cancer throughout the world, and the geographic patterns are very similar for men and women. There is a 10-fold variation in CRC incidence rates in both sexes, worldwide. Australia/New Zealand has the highest age-standardized rates of CRC incidence per 100,000 individuals, with 44.8 for men and 32.2 for women. West Africa has the lowest rates, with 4.5 for men and 3.8 for women per 100,000 individuals. Worldwide mortality from CRC is lower than its worldwide morbidity, with 694,000 deaths, representing 8.5% of all malignancies. There are more deaths from CRC (52%) in the less developed regions of the world, reflecting a lower survival rate for this malignancy in those regions. There is less variability in CRC mortality rates (six-fold in men, four-fold in women) than in morbidity rates across the world. The highest mortality rates estimated for both sexes are in Central and Eastern Europe, with a rate of 20.3 per 100,000 for men and 11.7 per 100,000 for women. The lowest rates are in West Africa, with 3.5 for men and 3 for women.1
On the American continent, a wide variation in mortality from CRC was also observed in 2012. There were 112,024 deaths, 55,002 of which were in women and 57,022 in men. Uruguay had the highest mortality rate, at 15.7 per 100,000 persons, whereas Guatemala had the lowest mortality rate, at 2.9. In that same year in Mexico, there were 4,694 deaths from CRC, 2,166 of which were in women and 2,528 in men. The mortality rate was 4.8 per 100,000 individuals.2
In 2002 in Mexico, there were 108,064 new cases with a histopathologic diagnosis of cancer, of which 3,791 (3.5%) were due to CRC. Of those cases, 2,491 (2.3%) corresponded to colon cancer and 1,300 (1.2%) to rectal cancer, placing this tumor among the 10 most prevalent causes of morbidity from malignancies in the country. A direct relationship between new cases of colorectal cancer and age has been observed. Almost half of the new cases occur in the population ≥ 60 years of age. Mexican mortality rates due to colon cancer have increased considerably in the last three decades. In 1985, there were 1,004 deaths in both sexes, and in 2002, there were 2,178 deaths. In 2002, 58,612 cancer deaths were registered, of which 2,602 (4.43%) were from CRC. Of those cases, 2,178 were due to colon cancer and 424 were ascribed to rectal cancer, representing a rate of 2.1 and 0.4 per 100,000 individuals, respectively. There was a slight predominance of colon cancer in females (51 vs 49%) and a predominance of rectal cancer in males (53 vs 46%).3
There are no Mexican studies investigating trends in mortality and the risk of dying from CRC in relation to educational level and socioeconomic region. Thus, we believe it would be useful to have an analysis of mortality trends by state and by socioeconomic region and to establish the relative risk between both educational level and socioeconomic region and mortality due to CRC.
The aims of this study were to determine mortality trends by socioeconomic region and by state, and to establish the relative risk between both educational level and socioeconomic region and the mortality from CRC within the time frame of 2000-2012.
Materials and methodsAn ecologic study design was utilized. Mortality records associated with CRC from 2000-2012 were obtained from the Health Information Administration of the Mexican Health Department.4 This information is generated by the National Institute of Statistics and Geography (INEGI, Spanish acronym) and it is collected from the death certificates issued nationwide. All individual records of mortality in which the basic cause of death was CRC within the time frame of 2000 and 2012 were included in the study. The codes of the International Classification of Diseases, tenth revision, were identified.5 They corresponded to the basic cause of death from CRC (C18-C18.9, C19-C20, C21-C21.8).
Raw and age-adjusted mortality rates nationwide per 100,000 inhabitants were obtained, using the world population as the standard population.6,7 Age-adjusted mortality rates per 100,000 inhabitants from each state and from each of the 7 socioeconomic regions established by the INEGI (table 1) were also obtained.8 The national population, estimated by the National Population Council for 2000-2012,9 was used for the rate adjustment. The relative risk (RR) and 95% confidence interval (CI) were obtained through the Poisson regression to determine the strength of association of the educational level and each of the seven socioeconomic regions with CRC mortality rates.
The socioeconomic regions of Mexico.
| Socioeconomic regions | States |
|---|---|
| 1 | Chiapas, Guerrero, Oaxaca |
| 2 | Campeche, Hidalgo, Puebla, San Luis Potosí, Tabasco, Veracruz |
| 3 | Durango, Guanajuato, Michoacán, Tlaxcala, Zacatecas |
| 4 | Colima, Estado de México, Morelos, Nayarit, Querétaro, Quintana Roo, Sinaloa, Yucatán |
| 5 | Baja California, Baja California Sur, Chihuahua, Sonora, Tamaulipas |
| 6 | Aguascalientes, Coahuila, Jalisco, Nuevo León |
| 7 | Mexico City |
Source: National Institute of Statistics and Geography (INEGI).
The 7 socioeconomic regional categories for Mexico have been defined by the INEGI. The differences observed in the social and economic conditions of the population throughout Mexico are presented according to the XII General Population and Housing Census. The 7 socioeconomic regions include the 31 states and Mexico City, and are formed based on indicators related to well-being, such as education, occupation, health, housing, and employment. On average, the states classified in the same region have similar characteristics, in other words, they are homogeneous, whereas the regions differ from one another. According to the indicators used, the socioeconomic conditions advance from region 1, the least favorable, to region 7, the most favorable.
The methodology used to determine the regions formed strata with minimal variance, grouping together the elements that were most alike, following an established similarity criterion. In this manner, each region could be distinguished from the other. Among the techniques used were Mahalanobis distances and a combination of factorial analysis and the k-means clustering algorithm.8
The Poisson regression model was chosen to determine the strength of association of the socioeconomic regions of residence and the educational levels with CRC mortality, because as a dependent variable, the number of deaths had a Poisson distribution that took positive whole values. The Poisson regression is equivalent to a logarithmic regression of mortality rates. The exponential coefficients enabled the RR of dying to be estimated.10
The strength of association of educational level and each socioeconomic region with the CRC mortality rate was obtained by the Poisson regression through the 2001 Number Cruncher Statistical System program.11 The Epidat version 3.1 program was used to determine the age-adjusted mortality rates by state and socioeconomic region.
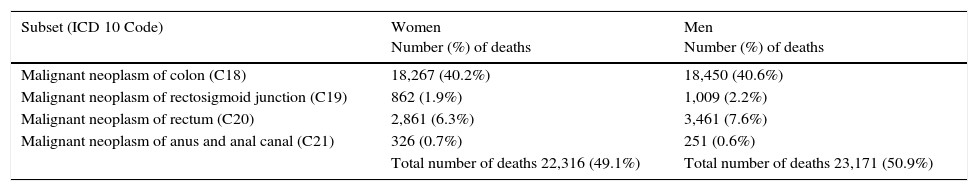
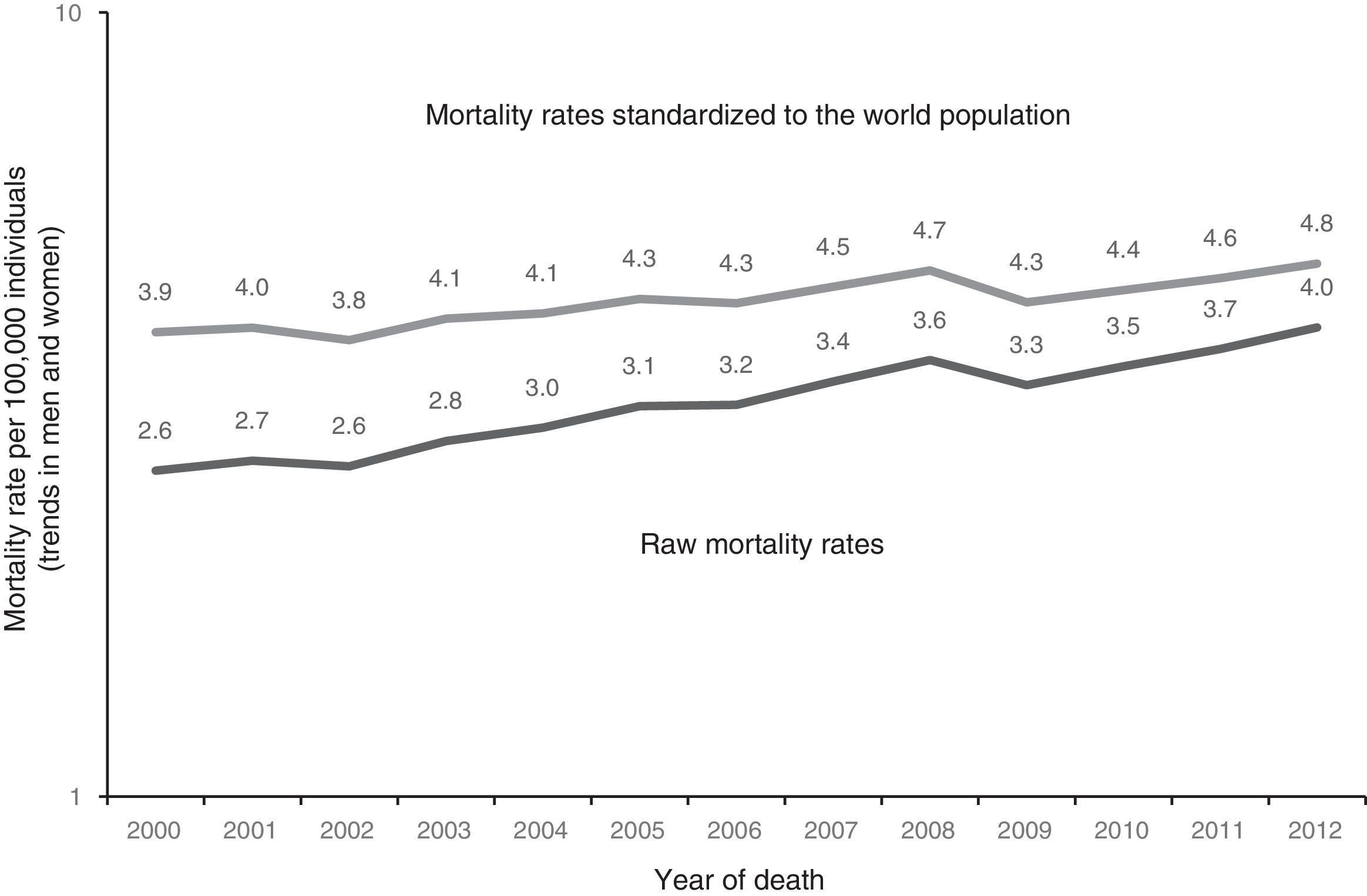
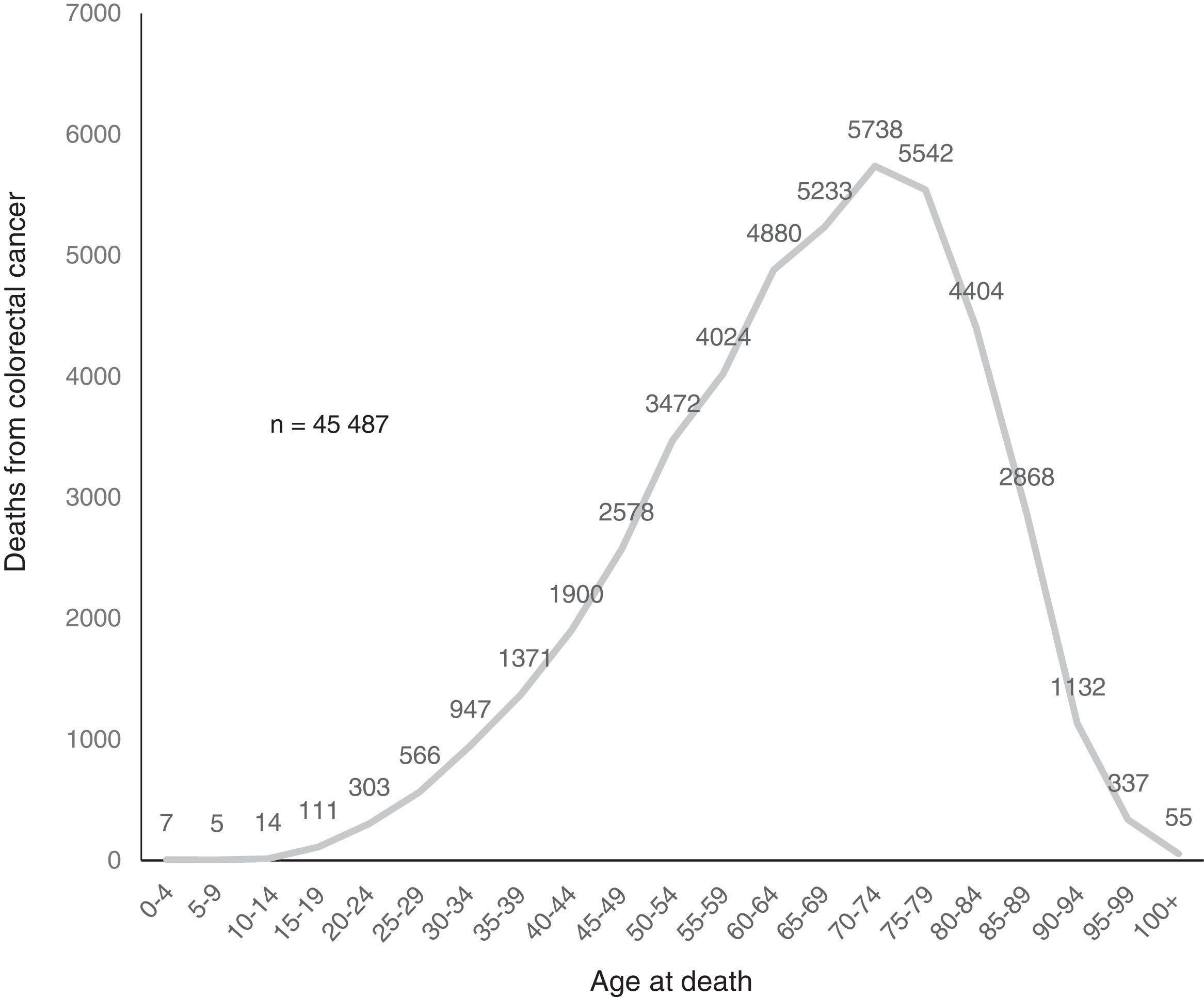
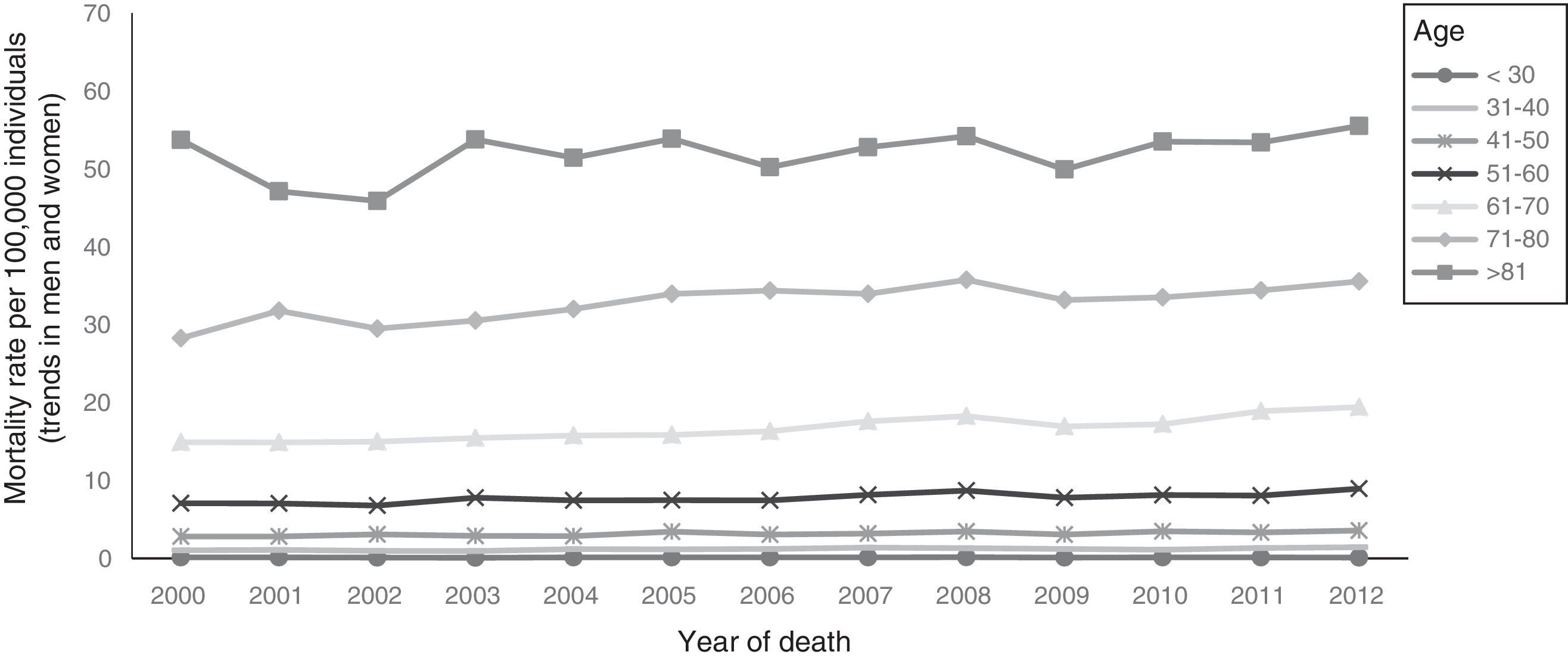
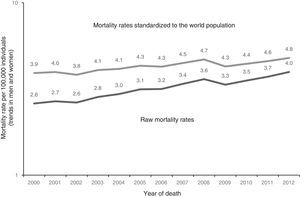
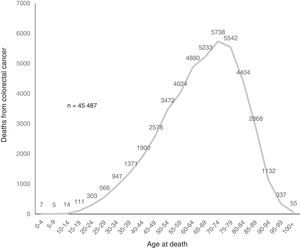
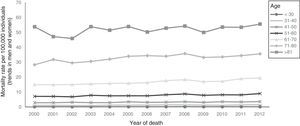
ResultsIn Mexico, within the time frame of 2000 through 2012, 45,487 individuals died from CRC, of which 22,316 (49.1%) were women and 23,171 (50.9%) were men (table 2). During the study period, the adjusted-mortality rate for CRC increased from 3.9 to 4.8 per 100,000 individuals (fig. 1). Mortality from CRC increased notably with age. In the age group of 40 to 44 years, 1,900 (4.2%) individuals died from CRC, whereas in the group of 70 to 74 years, mortality reached its highest level, with 5,738 (12.6%) individuals (fig. 2). During the time frame of the study, mortality rates for CRC by age group increased in all groups except for the age group under 30 years. The highest mortality rate (per 100,000) was observed in the age group above 81 years (in 2000 it was 53.7 and in 2012 it was 55.5) (fig. 3).
Deaths from colorectal cancer by disease site. Mexico, 2000-2012.
| Subset (ICD 10 Code) | Women Number (%) of deaths | Men Number (%) of deaths |
|---|---|---|
| Malignant neoplasm of colon (C18) | 18,267 (40.2%) | 18,450 (40.6%) |
| Malignant neoplasm of rectosigmoid junction (C19) | 862 (1.9%) | 1,009 (2.2%) |
| Malignant neoplasm of rectum (C20) | 2,861 (6.3%) | 3,461 (7.6%) |
| Malignant neoplasm of anus and anal canal (C21) | 326 (0.7%) | 251 (0.6%) |
| Total number of deaths 22,316 (49.1%) | Total number of deaths 23,171 (50.9%) |
Mortality from colorectal cancer in Mexico, 2000-2012. Raw mortality rate per 100,000 inhabitants. Direct age-adjusted rate per 100,000 inhabitants standardized to the world population. Raw mortality rates (trends in men and women). Standardized mortality rates (trends in men and women).
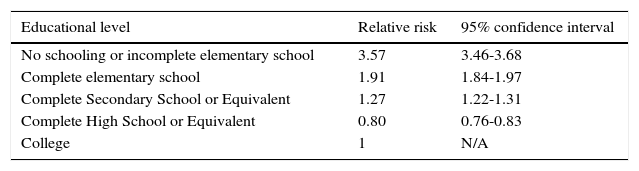
The individuals that died from CRC had a higher risk of dying if they had a lower educational level. Individuals with no schooling or incomplete elementary school had a RR of dying of 3.57, 95% CI: 3.46-3.68, whereas individuals with a higher educational level had a lower risk of dying. Individuals that completed high school or its equivalent had a RR of 0.80, 95% CI: 0.76-0.83 (table 3).
Relative risk of dying from colorectal cancer according to educational level, and the 95% confidence interval (CI) according to the Poisson regression. Mexico, 2000-2012.
| Educational level | Relative risk | 95% confidence interval |
|---|---|---|
| No schooling or incomplete elementary school | 3.57 | 3.46-3.68 |
| Complete elementary school | 1.91 | 1.84-1.97 |
| Complete Secondary School or Equivalent | 1.27 | 1.22-1.31 |
| Complete High School or Equivalent | 0.80 | 0.76-0.83 |
| College | 1 | N/A |
Note: N/A: Not applicable.
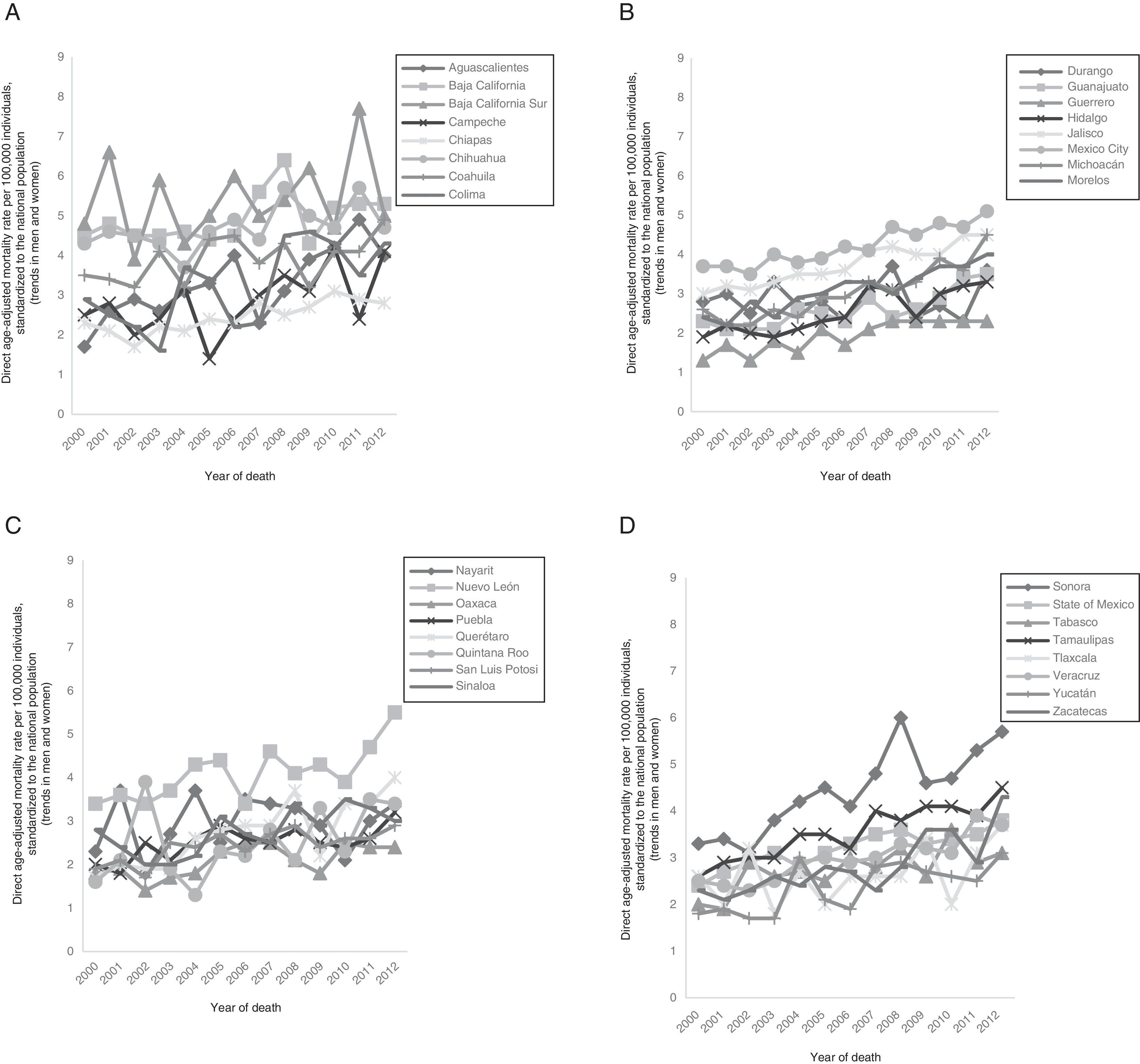
The Mexican states with the highest mortality from CRC in the years 2000-2012 were Baja California Sur (2000, 2001, 2003, 2005, 2006, 2009, 2011), Baja California (2002, 2004, 2007, 2008, 2010), and Sonora (2012). The mortality rate in 2000 in Baja California Sur was 4.8 and in 2011 it was 7.7. In 2002, the mortality rate in Baja California was 4.5 and in 2010 it was 5.2. In Sonora, the mortality rate was 5.7 in 2012 (fig. 4).
Within the study's time frame, the states with the lowest mortality from CRC were Guerrero (2000-2002, 2006, 2007, 2011, 2012), Colima (2003), Quintana Roo (2004), Campeche (2005), Oaxaca (2008-2009), and Tlaxcala (2010). In Guerrero in 2000, the CRC mortality rate was 1.3 and in 2012 it was 2.3. In Colima in 2003, it was 1.6; in Quintana Roo in 2004, it was 1.3; and in Campeche in 2005, it was 1.4. In 2008 and 2009 in Oaxaca, the mortality rate was 2.1 and 1.8, respectively, and in Tlaxcala in 2010, it was 2 (fig. 4).
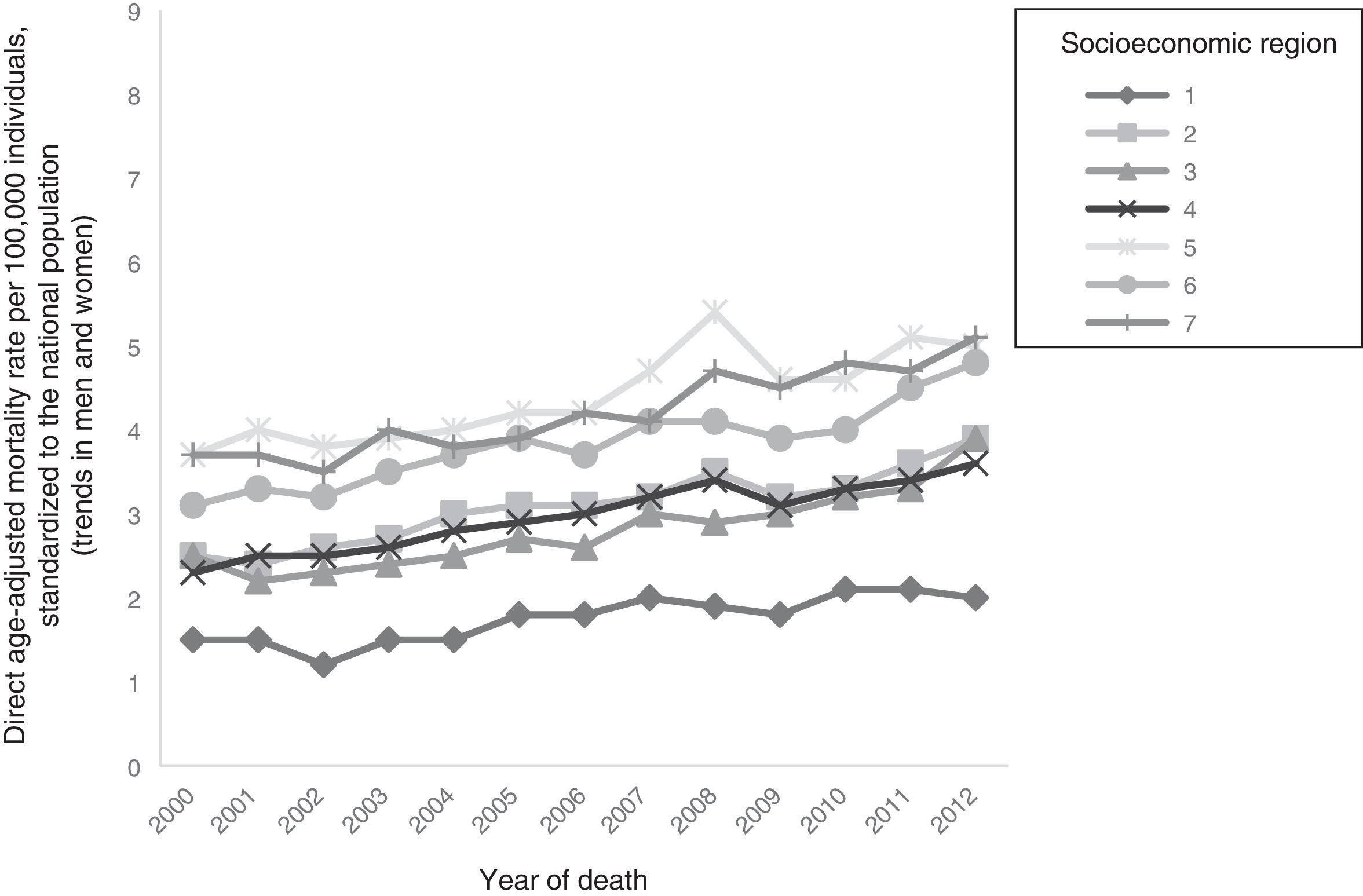
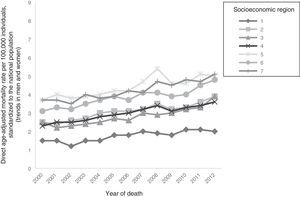
Socioeconomic regions with the highest mortality from CRC were region 5 (2001, 2002, 2004, 2005, 2007-2009, 2011) and region 7 (2003, 2010, 2012). Regions 5 and 7 had the highest mortality in 2000 and 2006. In 2001, region 5 had a mortality rate of 4 and in 2011 it was 5.1. In 2003 in region 7, mortality was 4 and in 2012, it was 5.1. In 2000 and 2006, regions 5 and 7 had mortality rates of 3.7 and 4.2, respectively. During the study period, region 1 had the lowest mortality rate. It was 1.5 in 2000 and 2 in 2012 (fig. 5).
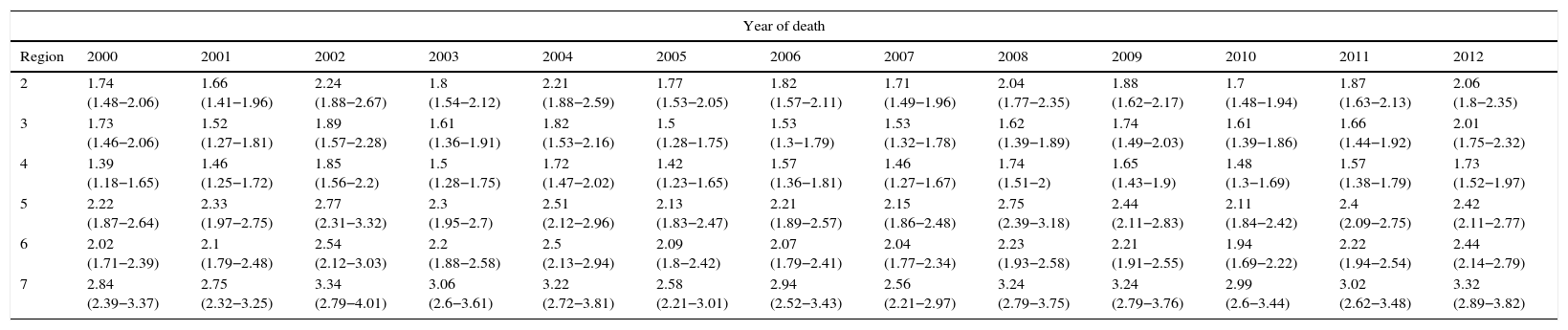
From 2000 to 2012, the risk of dying from CRC was higher in individuals residing in region 7. In 2000 in region 7, the RR was 2.84, with a 95% CI of 2.39-3.37, and in 2012 it was 3.32, with a 95% CI of 2.89-3.82 (table 4). The regions with the lowest strength of association with CRC mortality were region 4 (2000-2005, 2007, 2009-2012) and region 3 (2006, 2008). In 2000, region 4 had a RR of 1.39, with a 95% CI of 1.18-1.65, and in 2012 the RR was 1.73, with a 95% CI of 1.52-1.97. In region 3, the RR in 2006 was 1.53, with a 95% CI of 1.3-1.79, and in 2008 the RR was 1.62, with a 95% CI of 1.39-1.89 (table 4).
Relative risk of dying from colorectal cancer by socioeconomic region and the 95% confidence interval according to the Poisson Regression. Mexico, 2000-2012.
| Year of death | |||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Region | 2000 | 2001 | 2002 | 2003 | 2004 | 2005 | 2006 | 2007 | 2008 | 2009 | 2010 | 2011 | 2012 |
| 2 | 1.74 (1.48−2.06) | 1.66 (1.41−1.96) | 2.24 (1.88−2.67) | 1.8 (1.54−2.12) | 2.21 (1.88−2.59) | 1.77 (1.53−2.05) | 1.82 (1.57−2.11) | 1.71 (1.49−1.96) | 2.04 (1.77−2.35) | 1.88 (1.62−2.17) | 1.7 (1.48−1.94) | 1.87 (1.63−2.13) | 2.06 (1.8−2.35) |
| 3 | 1.73 (1.46−2.06) | 1.52 (1.27−1.81) | 1.89 (1.57−2.28) | 1.61 (1.36−1.91) | 1.82 (1.53−2.16) | 1.5 (1.28−1.75) | 1.53 (1.3−1.79) | 1.53 (1.32−1.78) | 1.62 (1.39−1.89) | 1.74 (1.49−2.03) | 1.61 (1.39−1.86) | 1.66 (1.44−1.92) | 2.01 (1.75−2.32) |
| 4 | 1.39 (1.18−1.65) | 1.46 (1.25−1.72) | 1.85 (1.56−2.2) | 1.5 (1.28−1.75) | 1.72 (1.47−2.02) | 1.42 (1.23−1.65) | 1.57 (1.36−1.81) | 1.46 (1.27−1.67) | 1.74 (1.51−2) | 1.65 (1.43−1.9) | 1.48 (1.3−1.69) | 1.57 (1.38−1.79) | 1.73 (1.52−1.97) |
| 5 | 2.22 (1.87−2.64) | 2.33 (1.97−2.75) | 2.77 (2.31−3.32) | 2.3 (1.95−2.7) | 2.51 (2.12−2.96) | 2.13 (1.83−2.47) | 2.21 (1.89−2.57) | 2.15 (1.86−2.48) | 2.75 (2.39−3.18) | 2.44 (2.11−2.83) | 2.11 (1.84−2.42) | 2.4 (2.09−2.75) | 2.42 (2.11−2.77) |
| 6 | 2.02 (1.71−2.39) | 2.1 (1.79−2.48) | 2.54 (2.12−3.03) | 2.2 (1.88−2.58) | 2.5 (2.13−2.94) | 2.09 (1.8−2.42) | 2.07 (1.79−2.41) | 2.04 (1.77−2.34) | 2.23 (1.93−2.58) | 2.21 (1.91−2.55) | 1.94 (1.69−2.22) | 2.22 (1.94−2.54) | 2.44 (2.14−2.79) |
| 7 | 2.84 (2.39−3.37) | 2.75 (2.32−3.25) | 3.34 (2.79−4.01) | 3.06 (2.6−3.61) | 3.22 (2.72−3.81) | 2.58 (2.21−3.01) | 2.94 (2.52−3.43) | 2.56 (2.21−2.97) | 3.24 (2.79−3.75) | 3.24 (2.79−3.76) | 2.99 (2.6−3.44) | 3.02 (2.62−3.48) | 3.32 (2.89−3.82) |
Region 1 was used as a reference value for the Poisson regression.
In Mexico, there has been an upward trend in mortality rates from CRC over the past 3 decades. In 1985, CRC produced 1,004 deaths in both sexes,3 and the present study identified 4,641 deaths in 2012 from CRC. The age-adjusted mortality rate per 100,000 inhabitants increased from 3.9 to 4.8 during the years included in the study period (fig. 1). This same mortality trend has been reported in Central American, South American, and Eastern European countries, and perhaps can be explained by their limited health infrastructure and resources.12 A slight predominance of CRC mortality in men (50.9%) over women (49.1%) was observed (table 2). Factors that could be associated with a lower CRC mortality rate in women are a diet higher in fiber, increased physical activity, a lower body mass index, and a lower consumption of alcohol and tobacco. Hormone replacement therapy with estrogen and progestin at menopause has also been described as a factor that reduces the risk for CRC in women.13,14
An increase in mortality from CRC was identified in the older individuals of the study population. Cancer is generally a disease of aging.15 Morbidity and mortality of most cancers have been observed to increase with age up to 90 years and to decline thereafter.16 CRC is a disease caused by genetic alterations, which increase with age.17 The most well-known alterations in CRC are point mutations and insertion-deletion mutations.18
We found that Mexicans that died from CRC had a higher risk for death if they had a lower educational level, compared with those whose level of education was higher (table 3). Educational level is an indicator of health, given that persons with more schooling are more likely to be employed, have higher incomes, and consequently have greater well-being, directly affecting their health.19 In Mexico, the lack of a formal education has contributed to the prevalence of social inequality and poverty.20 A high level of education is related to low mortality and better health of the population.21 In Mexico, persons with no formal education or a low educational level are usually found in socially, geographically, and economically marginalized populations. The individuals in these populations have a greater possibility of dying from preventable cancers, such as CRC, because they do not receive opportune diagnosis and treatment, resulting in lower survival and higher mortality rates.22,23
Other studies have also found that patients with a low educational level are at a greater risk for CRC. Doubeni et al. found that patients with fewer than 12 years of schooling had a higher risk for developing CRC (rectum: an incidence rate ratio [IRR] of 1.64, 95% CI of 1.35-1.98; left colon: an IRR of 1.58, 95% CI of 1.31-1.90; and right colon: an IRR of 1.27, 95% CI of 1.10-1.46).24
The socioeconomic regions with the highest mortality from CRC were regions 5 and 7 (fig. 5), and the region with the highest risk of dying from CRC was region 7 (table 4), which corresponds to Mexico City. This region has the most favorable economic conditions of the country. Factors that have been associated with CRC are age, male sex, a family history of CRC, diabetes, obesity, physical inactivity, smoking, heavy alcohol consumption, a diet high in red and processed meats, and inadequate intake of fruits and vegetables.25,26 Factors that may be related to an increased risk of dying from CRC in Mexico City are obesity, physical inactivity, diabetes mellitus, and smoking. According to the National Health and Nutrition Examination Survey,27 Mexico City has the highest percentage in the country of overweight (39.9%) and obesity (33.9%). In addition, a high percentage of the population is sedentary, 82% of whom are female and 71% male.28 Mexico City also has the highest rates of morbidity and mortality for diabetes mellitus29 and the highest prevalence of youth smoking in the country, at 20.2%, with a 95% CI of 16.3-24.1.30
There is no specific program for CRC in Mexico. Such a program for the prevention and treatment of CRC is necessary, given that the screening programs in individuals at high risk for CRC that have been implemented have been shown to be cost-effective strategies. Due to the slow development of CRC, there is significant potential for reducing the burden of disease through early detection and removal of precancerous lesions in the early stages of CRC.31 Some studies have shown that the detection of fecal occult blood reduces mortality from CRC by 15-33% and that sigmoidoscopy and colonoscopy reduce mortality by 40% and 68%, respectively.32 These diagnostic tests have been recommended by expert committees and implemented in CRC prevention programs in Germany, Finland, and the United States.31
ConclusionsWithin the time frame of the present study, 45,487 individuals died due to CRC in Mexico. Age-adjusted CRC mortality rates per 100,000 inhabitants increased from 3.9 to 4.8 between 2000 and 2012, using the world population age distribution as the standard. Death predominated in men over women, with 23,171 (50.9%) and 22,316 cases (41.9%), respectively. Individuals with no schooling or incomplete elementary school had a higher risk of dying (RR 3.57, 95% CI: 3.46-3.68). The states with the highest mortality from CRC in the study period were Baja California Sur, Baja California, and Sonora. The risk of dying from CRC was highest in region 7.
Ethical responsibilitiesProtection of human and animal subjectsThe authors declare that no experiments were performed on humans or animals for this study.
Confidentiality of dataThe authors declare that no patient data appear in this article.
Right to privacy and informed consentThe authors declare that no patient data appear in this article.
Conflict of interestThe authors declare that there is no conflict of interest.
Please cite this article as: Sánchez-Barriga JJ. Tendencias de mortalidad y riesgo de muerte por cáncer colorrectal en las 7 regiones socioeconómicas de México, 2000-2012. Revista de Gastroenterología de México. 2017;82:217–225.