Normally, the bile ducts are sterile, but up to 4.2% of healthy persons can present with positive cultures. Certain circumstances favor that situation, such as gallstones or biliary tree manipulation. The aim of the present study was to determine the factors that influence the presence of bacteriobilia, as well as its implications for clinical practice.
Materials and methodsA prospective study was conducted on bile cultures from patients that underwent cholecystectomy at our hospital center within the time frame of 2013 to 2015.
ResultsThe study included 196 patients (42.3% women and 57.7% men) that underwent either open or laparoscopic cholecystectomy and in whom bile fluid samples were taken. The clinical, epidemiologic, and laboratory test characteristics of the patients were analyzed, as well as the surgical indication (urgent surgery or programmed surgery). With respect to microbiology, 47% of the bile cultures were positive: 56.5% presented with one microorganism, 25% with two, and 18.5% with three or more.
ConclusionMicrobiologic bile analysis should not be systematically performed, given that its result is relevant only in cases that present with demonstrated risk factors. However, in those cases, said analysis is essential to establish adequate antibiotic treatment, in relation to activity spectrum and duration, to prevent complications and an increase in microbial resistance.
Las vías biliares son normalmente estériles, aunque puede existir cultivo positivo hasta en un 4,2% de las personas sanas. Existen ciertas circunstancias que lo favorecen como pueden ser las litiasis o la manipulación de la vía biliar. El objetivo del estudio fue determinar los factores que influyen en la presencia de bacteriobilia, así como su implicación en la práctica clínica.
Material y métodosEstudio prospectivo de los cultivos de bilis obtenidos de los pacientes colecistectomizados en nuestro centro desde 2013 a 2015.
ResultadosSe recogieron un total de 196 pacientes, 42,3% mujeres y 57,7% hombres a los que se había realizado colecistectomía tanto abierta como laparoscópica tomando muestra del líquido biliar. Se analizaron las características clínicas, epidemiológicas y analíticas de los pacientes, así como la indicación quirúrgica (cirugía urgente o programada). Respecto a la microbiología en un 47% los cultivos de bilis recogidos fueron positivos: 56,5% con un microorganismo, 25% con dos y 18,5% con tres o más. También se incluyeron los antibióticos empleados tanto para tratamiento como para profilaxis.
ConclusiónEl análisis de la microbiología de la bilis no debería realizarse de forma sistemática, ya que solamente en casos en los que se demuestren los factores de riesgo estudiados su resultado puede llegar a ser relevante. En estos mismos casos también resulta imprescindible para establecer un tratamiento antibiótico adecuado tanto en lo referente al espectro como a la duración del mismo, con el fin de evitar complicaciones y el aumento de resistencias.
Biliary tree pathology, especially that secondary to infectious processes, is one of the main causes of emergency room consultations. Up to 20% of hospital admissions are related to acute cholecystitis, pancreatitis, choledocholithiasis, or cholangitis.1
Normally, the bile ducts are sterile, thanks to different anatomic mechanisms (sphincter of Oddi, hepatocyte cell junctions, Kupffer cells) and physiologic mechanisms, such as bile composition and flow, given that bile salts are bacteriostatic and limit the translocation of bacterial endotoxins.2
Even so, bacteriobilia can be detected in almost 4.2% of healthy persons.3 It is favored by certain circumstances, such as age, previous biliary tract manipulation, or lithiasis. Microorganisms enter the biliary tree through various mechanisms: the ascending route from the duodenum, the portal venous system, the periductal lymphatic route, or by way of hepatic secretion.
The aim of our study was to describe the risk factors for bacteriobilia, its relation to the severity of clinical symptoms, and whether the presence of the isolated microorganisms impact disease progression.
Materials and methodsA descriptive, prospective study was conducted on the bile cultures and characteristics of the patients that underwent cholecystectomy at our service, within the time frame of May 2013 to February 2015.
The inclusion criteria were patients 18 years of age or older, that were diagnosed with symptomatic gallstones (from simple biliary colic to acute cholecystitis) and indicated for programmed or emergency cholecystectomy, either as an open or laparoscopic procedure.
The exclusion criteria were patients diagnosed with cholangitis, patients that underwent cholecystectomy during the Whipple procedure for pancreatic neoplasias or biliary tract tumors, patients that underwent cholecystectomy due to gallbladder polyps, and patients that underwent percutaneous cholecystectomy.
Samples were taken intraoperatively, and within 2hours were sent to the Microbiology Service for bacteriologic culture. They were processed, following standardized laboratory protocols, and bacterial identification and sensitivity studies were carried out utilizing the Vitek 2 (bioMérieux®) and/or Phoenix (Becton Dickinson®) automated systems.
The epidemiologic variables analyzed were: sex, age, previous hospitalization, comorbidity, and proton pump inhibitor (PPI) use. The clinical variables were: diagnosis, severity grade, performance or not of endoscopic retrograde cholangiopancreatography (ERCP), type of approach (open/laparoscopic), surgical biliary tree examination or intraoperative cholangiography, pathologic anatomy of the gallbladder, postoperative complications, days of postoperative hospital stay, and postoperative deaths. The laboratory variables were: maximum alkaline phosphatase (ALP) value, bilirubin, GGT, AST, ALT, C-reactive protein (CRP), and leukocytes. The microbiologic variables were: antibiotic (ATB) use during the previous 6 months, ATB use upon admission, prophylactic ATB use, and isolated microorganisms.
The continuous variables were presented as median (interquartile range) and the qualitative variables as frequency (percentage). The categorical variables were compared using the chi-square test and the continuous variables with the Mann-Whitney U test. Logistic regression that included the statistically significant preoperative risk factor variables was employed for the multivariate analysis. Thus, odds ratios were analyzed, keeping in mind that a statistically significant odds ratio > 1 indicated an independent risk factor, whereas if it was not significant, it merely expressed a trend.
Statistical analysisThe SPSS® version 20 program (IBM, Armonk, New York, USA) was employed for the statistical analysis and statistical significance was set at a p<0.05.
Ethical considerationsThe Ethics Committee for Research with Medications (CEIm, the Spanish acronym) of our hospital approved the present study. Because the collection of the bile samples from the cholecystectomies was not an action that modified the indication for or performance of the procedure, obtaining informed consent from the study patients was not necessary.
ResultsBile samples from 196 patients (83 women [42.3%] and 113 men [57.7%]) were analyzed. The mean patient age was 61 years. The majority of the study patients underwent programmed laparoscopic procedures.
The median postoperative hospital stay was 3 days. Complications included 2 cases of bile duct fistula (1%) and 6 cases of abdominal collections (3.1%). Five patients died (2.6%).
Regarding the pathologic anatomy of the gallbladder, 80% of the cases had signs of acute cholecystitis, in both the programmed surgeries and the emergency interventions. There were no cases of neoplasia of the gallbladder. No significant correlation was found during the study between the microbiologic results and the pathologic anatomy.
With respect to ATB treatment: 91 patients (46%) had undergone some type of ATB treatment during the 6 months prior to surgery, related or not to biliary tree pathology. The 54 patients (27.6%) admitted to the hospital that underwent emergency surgery due to acute cholecystitis received ATB therapy as part of their treatment during hospitalization and the 142 patients (72.4%) that underwent programmed surgery received prophylactic ATB therapy (2g of cefazolin) 30min before surgery. The mean duration of ATB therapy for cholecystitis was 6 days. The ATBs most widely used as treatment were: piperacillin/tazobactam (77.8%), amoxicillin/clavulanic acid (14.8%), ertapenem (3.7%), and ciprofloxacin plus metronidazole (3.7%) in the patients allergic to penicillin.
Bile cultures were positive in 92 cases (47%): 52 (56.5%) with one microorganism, 23 (25%) with two microorganisms, and 17 (18.5%) with three or more microorganisms. A total of 167 microorganisms were isolated. The majority were Gram-negative bacilli (60.5%), most from the Enterobacteriaceae family (91/54.5%). Escherichia coli was the most frequent microorganism (40/24%), followed by Klebsiella spp. (21/12.5%).
A blood culture was ordered on 18 occasions (19.5%), in the patients with a positive bile culture. Growth was detected in 6 of them, but only two were considered significant (2.1%), with growth of the microorganism isolated in bile.
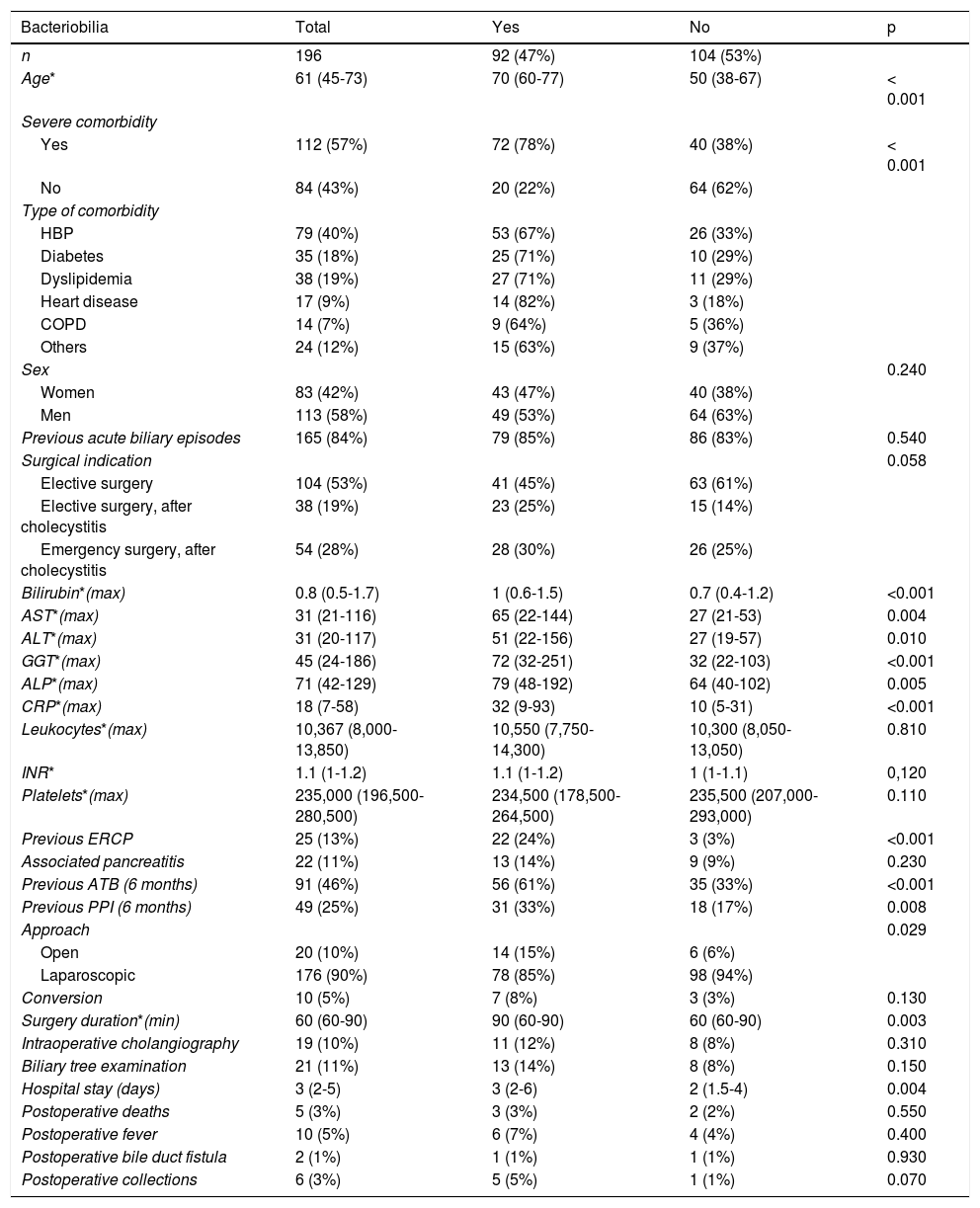
Table 1 shows the variables related to a positive or negative bile culture and whether or not there was statistical significance. According to those data, the factors associated with bacteriobilia were: advanced age (between 60 and 77 years), the presence of a severe comorbidity, higher levels of bilirubin, AST, ALT, GGT, ALP, and CRP, previous ERCP, previous ATB use (6 months prior to surgery), open surgical procedure, longer surgery duration, and longer postoperative hospital stay.
Epidemiologic, clinical, surgical, and laboratory test characteristics of the study sample.
| Bacteriobilia | Total | Yes | No | p |
|---|---|---|---|---|
| n | 196 | 92 (47%) | 104 (53%) | |
| Age* | 61 (45-73) | 70 (60-77) | 50 (38-67) | < 0.001 |
| Severe comorbidity | ||||
| Yes | 112 (57%) | 72 (78%) | 40 (38%) | < 0.001 |
| No | 84 (43%) | 20 (22%) | 64 (62%) | |
| Type of comorbidity | ||||
| HBP | 79 (40%) | 53 (67%) | 26 (33%) | |
| Diabetes | 35 (18%) | 25 (71%) | 10 (29%) | |
| Dyslipidemia | 38 (19%) | 27 (71%) | 11 (29%) | |
| Heart disease | 17 (9%) | 14 (82%) | 3 (18%) | |
| COPD | 14 (7%) | 9 (64%) | 5 (36%) | |
| Others | 24 (12%) | 15 (63%) | 9 (37%) | |
| Sex | 0.240 | |||
| Women | 83 (42%) | 43 (47%) | 40 (38%) | |
| Men | 113 (58%) | 49 (53%) | 64 (63%) | |
| Previous acute biliary episodes | 165 (84%) | 79 (85%) | 86 (83%) | 0.540 |
| Surgical indication | 0.058 | |||
| Elective surgery | 104 (53%) | 41 (45%) | 63 (61%) | |
| Elective surgery, after cholecystitis | 38 (19%) | 23 (25%) | 15 (14%) | |
| Emergency surgery, after cholecystitis | 54 (28%) | 28 (30%) | 26 (25%) | |
| Bilirubin*(max) | 0.8 (0.5-1.7) | 1 (0.6-1.5) | 0.7 (0.4-1.2) | <0.001 |
| AST*(max) | 31 (21-116) | 65 (22-144) | 27 (21-53) | 0.004 |
| ALT*(max) | 31 (20-117) | 51 (22-156) | 27 (19-57) | 0.010 |
| GGT*(max) | 45 (24-186) | 72 (32-251) | 32 (22-103) | <0.001 |
| ALP*(max) | 71 (42-129) | 79 (48-192) | 64 (40-102) | 0.005 |
| CRP*(max) | 18 (7-58) | 32 (9-93) | 10 (5-31) | <0.001 |
| Leukocytes*(max) | 10,367 (8,000-13,850) | 10,550 (7,750-14,300) | 10,300 (8,050-13,050) | 0.810 |
| INR* | 1.1 (1-1.2) | 1.1 (1-1.2) | 1 (1-1.1) | 0,120 |
| Platelets*(max) | 235,000 (196,500-280,500) | 234,500 (178,500-264,500) | 235,500 (207,000-293,000) | 0.110 |
| Previous ERCP | 25 (13%) | 22 (24%) | 3 (3%) | <0.001 |
| Associated pancreatitis | 22 (11%) | 13 (14%) | 9 (9%) | 0.230 |
| Previous ATB (6 months) | 91 (46%) | 56 (61%) | 35 (33%) | <0.001 |
| Previous PPI (6 months) | 49 (25%) | 31 (33%) | 18 (17%) | 0.008 |
| Approach | 0.029 | |||
| Open | 20 (10%) | 14 (15%) | 6 (6%) | |
| Laparoscopic | 176 (90%) | 78 (85%) | 98 (94%) | |
| Conversion | 10 (5%) | 7 (8%) | 3 (3%) | 0.130 |
| Surgery duration*(min) | 60 (60-90) | 90 (60-90) | 60 (60-90) | 0.003 |
| Intraoperative cholangiography | 19 (10%) | 11 (12%) | 8 (8%) | 0.310 |
| Biliary tree examination | 21 (11%) | 13 (14%) | 8 (8%) | 0.150 |
| Hospital stay (days) | 3 (2-5) | 3 (2-6) | 2 (1.5-4) | 0.004 |
| Postoperative deaths | 5 (3%) | 3 (3%) | 2 (2%) | 0.550 |
| Postoperative fever | 10 (5%) | 6 (7%) | 4 (4%) | 0.400 |
| Postoperative bile duct fistula | 2 (1%) | 1 (1%) | 1 (1%) | 0.930 |
| Postoperative collections | 6 (3%) | 5 (5%) | 1 (1%) | 0.070 |
ALP: alkaline phosphatase; ALT: alanine transaminase; AST: aspartate aminotransferase; ATB: antibiotic; COPD: chronic obstructive pulmonary disease; CRP: C-reactive protein; ERCP: endoscopic retrograde cholangiopancreatography; GGT: gamma-glutamyl transferase; HBP: high blood pressure; INR: international normalized ratio; PPI: proton pump inhibitor.
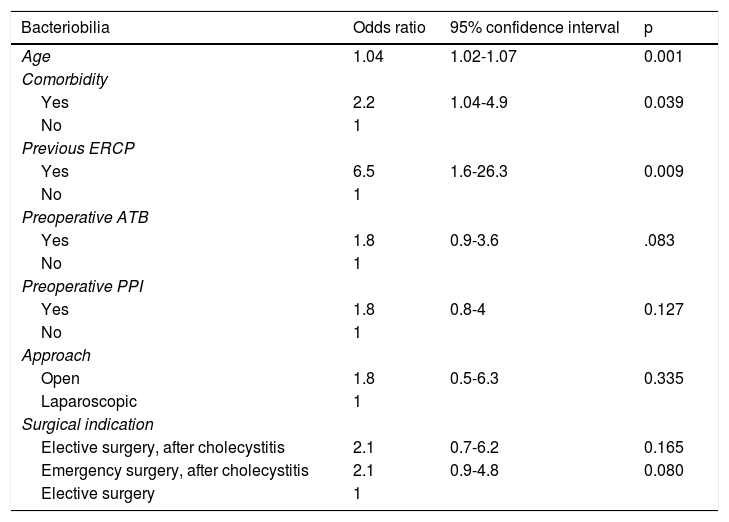
A logistic regression analysis was then performed on the most relevant preoperative variables (Table 2) and statistically significant differences were obtained in relation to advanced age, the presence of a comorbidity, and previous ERCP, which was the most important variable (OR of 6.5). Previous ATB use and indication for emergency surgery due to cholecystitis almost reached statistical significance, showing a marked trend.
Logistic regression: preoperative risk factors.
| Bacteriobilia | Odds ratio | 95% confidence interval | p |
|---|---|---|---|
| Age | 1.04 | 1.02-1.07 | 0.001 |
| Comorbidity | |||
| Yes | 2.2 | 1.04-4.9 | 0.039 |
| No | 1 | ||
| Previous ERCP | |||
| Yes | 6.5 | 1.6-26.3 | 0.009 |
| No | 1 | ||
| Preoperative ATB | |||
| Yes | 1.8 | 0.9-3.6 | .083 |
| No | 1 | ||
| Preoperative PPI | |||
| Yes | 1.8 | 0.8-4 | 0.127 |
| No | 1 | ||
| Approach | |||
| Open | 1.8 | 0.5-6.3 | 0.335 |
| Laparoscopic | 1 | ||
| Surgical indication | |||
| Elective surgery, after cholecystitis | 2.1 | 0.7-6.2 | 0.165 |
| Emergency surgery, after cholecystitis | 2.1 | 0.9-4.8 | 0.080 |
| Elective surgery | 1 |
ATB: antibiotic; ERCP: endoscopic retrograde cholangiopancreatography: PPI: proton pump inhibitor.
The clinical consequences of bacterial isolation in bile continue to be a subject of debate. The results from studies in the literature on the risk factors for developing bacteriobilia are heterogenous and often contrasting.4 In some articles, the presence of bacteriobilia has been related to the development of more severe infections or processes. For example, in their studies, Darcahi et al.5 and Galili et al.6 described an association between bacteriobilia and the development of infectious complications in patients with acute cholecystitis. A relation was also found between bacteriobilia in the context of obstructive jaundice and the risk for a postoperative infectious complication in the study by Namias et al.7 In addition, different authors have reported that advanced-age patients present with more severe disease.8
In contrast, authors of other studies have found no relation between the presence of bacteriobilia and later infectious complications.9,10 The work of Park et al.11 stands out in that regard, in which they concluded that more than half of the microorganisms isolated in bile cultures could not be considered pathogens, especially the Gram-positive ones.
The factors related to the increased presence of bacteriobilia, most widely described in the literature are:
- Previous biliary tree manipulation (ERCP).12
- Bile duct stones.13,14
- The presence of comorbidities or a high American Society of Anesthesiologists (ASA) classification.
- Male sex.15
- Advanced age (> 60 years), which has also been associated with a greater risk for bacteriobilia and a worse later progression, possibly related to an immune response alteration.16,17
- Patients with biliary obstruction that present with fever, a palpable gallbladder upon physical examination, leukocytosis, elevated serum ALP, or patients that have developed bacteremia.18
We employed univariate statistical techniques in our study, whose results concurred with some of those factors, one of which was advanced age (> 60 years). Our patients with positive bile cultures had a median age of 70 years, whereas the cases with negative cultures had a median age of 50 years. There was also a clear relation between the presence of comorbidities and positive cultures. In contrast, the sex of the patients in our study was not a risk factor for presenting with bacteriobilia.
With respect to the form of biliary tract pathology, there was a greater presence of positive cultures in the cases with higher levels of bilirubin, transaminases, and CRP, reflecting their relation to the clinical pictures of the patients that presented with biliary obstruction. However, we found no significant association with having had previous acute episodes of biliary pain, even of pancreatitis. There was also no greater bacteriobilia in the cultures of the patients that underwent emergency surgery due to acute cholecystitis than in those that underwent programmed interventions. In contrast, open surgery and longer surgery duration, which were possible aspects of the more complex cases, were related to a greater presence of bacteriobilia.
Previous biliary tree manipulation through ERCP showed a direct relation to bacteriobilia, whereas intraoperative cholangiography and biliary tree examination did not reflect a higher number of positive cultures.
There were no statistically significant differences in the postoperative complications analyzed (fever, fistula, and abdominal collection) that were related to the presence of bacteriobilia. However, there were clinically relevant differences associated with postoperative intra-abdominal collections, in which there were 5-times more cases of positive bacteriobilia. Likewise, longer hospital stay (2 to 6 days) was also related to positive bile cultures, implying that the more complex cases were likely to have had longer periods of hospitalization. The fact that the complications were not statistically significant, even though they involved complex cases, could be due to their small number.
Both groups presented with similar mortality figures, with a total of 5 deaths, all related to patients with severe cholecystitis that underwent emergency surgery.
Both ATB use and PPI use during the 6 months prior to surgery were associated with increased bacteriobilia in the cultures.
In the multivariate study, advanced age, severe comorbidity, and previous ERCP were identified as independent risk factors for bacteriobilia. Previous biliary tree manipulation (ERCP) was the most important risk factor, with a 6-times higher risk for presenting with bacteriobilia, followed by severe comorbidity with a 2-times higher risk, and advanced age. ATB use during the 6 months prior to surgery and the indication for emergency surgery almost reached statistical significance, signifying a marked trend toward the presence of bacteriobilia in those situations.
Regarding the practical application of those data, upon reviewing the literature, we found that Herzog et al.19 recommend the systematic collection of bile samples for cultures during biliary tract surgery to better adapt antibiotic prophylaxis to local sensitivities. Likewise, when there are signs of infection, the importance of collecting samples for culture from the focus of infection must not be ignored, given the possible impact on the later adaptation of ATB treatment the patient may require.20,21
Other studies, such as the one by Troyano et al.,22 also recommend taking the results of the cultures into account, even if no association with the development of infections is found, especially in high-risk patients. However, authors like Park et al.,11 do not recommend routinely collecting samples for cultures, but rather reserving the practice for the cases in which there are data or suspicion of infection.
On the other hand, the importance of early treatment in biliary tract infections should be underlined, as well as the need to adapt the treatment spectrums of empirically administered ATBs,23,24 contemplating the culture results as soon as they are available, evaluating the conversion to oral agents whenever possible, and attempting to minimize the duration of ATB treatment.25,26
In conclusion, the recommendation to collect bile samples for culture in all biliary tree procedures cannot be generalized, but the practice could be justified in certain high-risk patients, especially those presenting with the demonstrated independent risk factors for increased bacteriobilia: advanced age, severe comorbidity, and previous ERCP. Thus, each patient must be analyzed individually to evaluate the benefits of obtaining a bile culture. In cases of important infections, bile cultures are essential for adapting both the spectrum and duration of antibiotic treatment, as much as possible, according to the results of the culture.
Financial disclosureNo financial support was received in relation to this study.
AuthorshipAll the authors participated in the study design, analysis and interpretation of the results, drafting of the article and its critical review, and approval of the final version.
Conflict of interestThe authors declare that there is no conflict of interest.
Please cite this article as: Granel-Villach L, Gil-Fortuño M, Fortea-Sanchis C, Gamón-Giner RL, Martínez-Ramos D, Escrig-Sos VJ. Factores que influyen en la microbiología del líquido biliar en los pacientes colecistectomizados. Revista de Gastroenterología de México. 2020;85:257–263.