Preoperative serum alpha-fetoprotein levels can have predictive value for hepatocellular carcinoma survival.
AimOur aim was to analyze the correlation between preoperative serum alpha-fetoprotein levels and survival, following the surgical treatment of hepatocellular carcinoma.
MethodsNineteen patients were prospectively followed (07/2005-01/2016). An ROC curve was created to determine the sensitivity and specificity of alpha-fetoprotein in relation to survival (Kaplan-Meier).
ResultsOf the 19 patients evaluated, 57.9% were men. The mean patient age was 68.1 ± 8.5 years and survival at 1, 3, and 5 years was 89.4, 55.9, and 55.9%. The alpha-fetoprotein cutoff point was 15.1 ng/ml (sensitivity 100%, specificity 99.23%). Preoperative alpha-fetoprotein levels below 15.1, 200, 400, and 463 ng/ml correlated with better 1 and 5-year survival rates than levels above 15.1, 200, 400, and 463 ng/ml (P<.05).
ConclusionsElevated preoperative serum alpha-fetoprotein levels have predictive value for hepatocellular carcinoma survival.
Los niveles séricos de alfafetoproteína (AFP) preoperatoria pueden tener valor predictivo para la sobrevida del hepatocarcinoma (HCC).
ObjetivoAnalizar la correlación entre los niveles séricos de AFP preoperatoria y la sobrevida posterior al tratamiento quirúrgico del HCC.
MétodosDiecinueve pacientes fueron seguidos prospectivamente (julio del 2005-enero del 2016). Se realizó una curva ROC para determinar la sensibilidad y la especificidad de la AFP con relación con la sobrevida (Kaplan-Meier).
ResultadosSe evaluó a 19 pacientes, 57.9% hombres, edad media 68.1 ± 8.5 años con sobrevida a 1, 3 y 5 años del 89.4, el 55.9 y el 55.9%. El punto de corte de AFP fue 15.1 ng/ml (sensibilidad 100%, especificidad 99.23%). Los niveles preoperatorios de AFP menores de 15.1, 200, 400 y 463 ng/ml correlacionaron con mejor sobrevida a 1 y 5 años que niveles mayores de AFP (p < 0.05).
ConclusionesLos niveles séricos preoperatorios elevados de AFP tienen valor predictivo en relación con la sobrevida de HCC.
Hepatocellular carcinoma (HCC) represents 4% of cancers diagnosed worldwide and it is the fifth most common cancer in the world.1 In Mexico, its incidence has increased over the past decades.2
Serum alfa-fetoprotein (AFP) is the most important marker for HCC diagnosis. Some experts regard AFP levels > 200 ng/ml as diagnostic for HCC, whereas others consider the figure to be AFP levels > 400 ng/ml.3 Elevated AFP levels have been linked to large bi-lobular lesions and portal vein thrombosis,4,5 and AFP levels have been reported to have predictive value for HCC survival and recurrence.4–6 However, there is no consensus on the value of preoperative AFP for predicting survival and recurrence after liver resection in HCC.
Five-year survival in HCC after a resection is 50-80%.4 In Mexico, the information on preoperative AFP values and survival in HCC patients after a liver resection is insufficient.2,7–10 Our aim was to analyze the correlation between preoperative serum AFP levels and 5-year survival after liver resection in HCC patients.
Materials and methodsA cohort of patients with HCC at our hospital that underwent resection as surgical treatment were prospectively followed within the time frame of July 2005 and January 2016, after prior authorization from the local ethics and research committee. Patients were excluded that underwent other surgical treatments (local ablation, chemoembolization, transplant, chemotherapy, and no treatment). Age, sex, body mass index, cirrhosis, viral hepatitis, Child-Pugh classification,10 and the model for end-stage liver disease (MELD) score were registered.10 The number of lesions, tumor size and location, and preoperative AFP level were determined. The patients were classified according to the Okuda and the Barcelona Clinic Liver Cancer (BCLC) staging systems.10
Intensive care unit stay, hospital stay, postoperative liver failure, and perioperative mortality were documented. Follow-up was conducted through outpatient consultations. Tumor recurrence was defined as the appearance of new radiologic lesions, and survival was calculated from the beginning of the patient's evaluation up to his or her death or follow-up loss.
Statistical analysisThe continuous variables were described through mean, standard deviation, and range and the categorical variables were described through frequency and percentage. A receiver operating characteristic (ROC) curve was plotted to determine the area under the curve, cut-off point, and sensitivity and specificity of preoperative AFP levels for survival in all the patients, calculated using the Kaplan-Meier estimator. In addition, the positive predictive value and negative predictive value of the ROC curve cut-off point were determined for all the patients. Survival in the patients with different preoperative AFP values (mean, ROC curve cut-off point, 200 ng/ml, and 400 ng/ml) were compared (log-rank, Mantel-Cox). Cox regression was carried out with the different AFP levels to determine the survival risk in those patients. Statistical significance was set at a p < 0.05.
ResultsFifty-two patients were diagnosed with HCC during the study period. Twelve of those patients received no treatment, 14 underwent radiofrequency ablation, 2 had transarterial chemoembolization, and 5 received chemotherapy (sorafenib), all of whom were excluded from the analysis. The study cohort was made up of the remaining 19 patients that underwent resection and 57.9% of them were men (n = 11). The mean age of the study patients was 68.1 ± 8.5 years (range: 44-81) and the mean body mass index was 26.4 ± 3.6kg/m2 (range: 18.5 - 33.3). A total of 26.3% (n = 5) of the patients presented with cirrhosis (Child-Pugh A, etiology: 2 patients with non-alcoholic steatohepatitis, 1 with alcoholic steatohepatitis, and one patient with hepatitis C and alcoholic steatohepatitis). Five patients (26.3%) had hepatitis C virus (4 without cirrhosis). The etiology of liver damage without cirrhosis in the remaining patients was determined in 8 of them (4 with nonalcoholic steatohepatitis and 4 with alcoholic steatohepatitis). The mean AFP level was 463.3 ± 1,057 ng/ml (range: 1.7-4002.4).
The mean lesion size was 6.6 ± 2.4cm (range: 2-10). Eighteen patients (94.7%) had a single tumor and 63.7% of the lesions were on the right side (n = 12). A total of 52.6% (n = 10) of the patients were classified as Okuda stage I and the mean MELD score was 7.6 ± 2.3 (range: 1-11). All the patients were classified as BCLC stage A.
Eleven patients (57.9%) required treatment in the intensive care unit (1.6 ± 1.9 days, range: 0-7). Mean hospital stay was 8.8 ± 4.9 days (range: 5-21). Three patients (15.7%) had transitory postoperative liver failure. One patient died due to postoperative liver failure and another from a cerebrovascular event. Four patients presented with recurrence (mean 6.8 ± 14.5 months, range: 11-50), resulting in the death of 2 of them, and one patient died from a cardiovascular event (25 months). The estimated overall survival was 55.1 ± 10 months (range: 35.3-74.8) and the actuarial overall survival at one year (13 patients), 3 years (6 patients), and 5 years (6 patients) was 89.4, 55.9, and 55.9%, respectively.
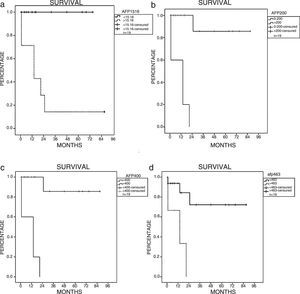
The ROC curve established an area under the curve of 0.987 (95% CI: 0.947-1.0) (p = 0.001), with sensitivity of 100% and specificity of 99.2% for a cutoff point of 15.1 ng/ml, a positive predictive value of 100%, and a negative predictive value of 85.7%. Patients with preoperative AFP levels < 15.1 ng/ml (n = 12) had better survival at one, 3, and 5 years (100%) (mean and median survival: 29 and 15.5 months, respectively) than those with AFP levels > 15.1 ng/ml (n = 7) (71.4, 14.2, and 14.2%; mean and median survival: 23.2 and 14 months, respectively) (p = 0.001, log-rank) (fig. 1A). The patients with preoperative AFP levels < 200 ng/ml (n = 14) (mean and median survival: 32.9 and 205 months, respectively) had a better survival at one, 3, and 5 years (100 and 85.7% at 3 and 5 years) than those with AFP levels > 200 ng/ml (n = 5) (mean and median survival: 10.2 and 14 months, respectively) (60 and 0%, respectively) (p = 0.0001, log-rank) (fig. 1B). Likewise, the patients with preoperative AFP levels < 400ml (n = 14) (mean and median survival: 32.9 and 205 months, respectively) and with levels of < 463 ng/ml (n = 16) (mean and median survival: 29.7 and 15.5 months, respectively) had better survival at 1, 3, and 5 years (p = 0.0001 and p = 0.004, respectively, through log-rank) (fig. 1C and 1D), compared with the patients with preoperative AFP levels > 400 ng/ml (mean and median survival: 10.2 and 14 months, respectively) and with levels > 463 ng/ml (mean and median survival: 12 and 14 months, respectively). The Cox regression produced no significant differences between the different AFP levels (AFP > 15.16 ng/ml [p = 0.933], AFP > 200 ng/ml [p = 0.938], AFP > 400 ng/ml [p = 0.938], and AFP > 463 ng/ml [p = 0.584]).
A) Survival in relation to preoperative AFP of 15.1 ng/ml (p = 0.001). B) Survival in relation to preoperative AFP of 200 ng/ml (p = 0.0001). C) Survival in relation to preoperative AFP of 400 ng/ml (p = 0.0001). D) Survival in relation to preoperative AFP of 463 ng/ml (p = 0.004).
AFP: Alpha-fetoprotein.
Our results confirmed the relation of preoperative serum AFP levels to survival in patients that underwent liver resection as HCC treatment. The levels of AFP <15.1 ng/ml and other previously established ones had a statistically significant rate of survival above 5 years.
Different studies suggest the relation of an elevated preoperative serum AFP level to the prediction of recurrence, survival, and outcome in HCC.4–6 Tangkijvanich et al.5 concluded that AFP was useful in the diagnosis and prognosis of patients divided into groups of AFP < 20 ng/ml (normal), markedly elevated (20-399 ng/ml), and very elevated (> 400 ng/ml), with greater survival in the first 2 groups. Likewise, Wen-Jun et al.6 observed that those patients with serum AFP levels < 20 ng/ml had a lower recurrence rate at 2 years and an 18 to 24-month greater survival than the others. Li et al.4 corroborated the fact that liver resection for HCC had a better outcome if the AFP levels were low. Our results offer a cutoff point below 20 ng/ml, with sensitivity and specificity above 90%, and statistically significant differences in survival. The same occurred when the values were > 200 and 400 ng/ml, with no AFP value having greater statistical significance, indicating that the simple elevation of AFP above normal values suggests a worse outcome in those patients.
The relation of the preoperative value of AFP to outcome in patients with HCC has not been studied in Mexico. In 1997, Mondragón Sánchez et al.8 suggested that AFP levels had low sensitivity for diagnosing HCC. Ladrón-de-Guevara et al.7 described mean levels of AFP of 516 ng/ml in patients with HCC, without exploring its influence on outcome. Meza-Junco et al.10 found that 25.2% of patients had an AFP level > 40 ng/ml at diagnosis. Our group9 previously reported that patients that underwent liver resection had lower AFP levels than other patients, which led to the development of the present study.
ConclusionsPatients with preoperative AFP levels > 15 ng/ml that underwent liver resection as HCC treatment had a lower 5-year survival rate than the patients with AFP levels < 15 ng/ml. Those findings must be corroborated in other case series with different population characteristics.
Ethical disclosuresProtection of human and animal subjectsThe authors declare that no experiments were performed on humans or animals for this study.
Confidentiality of dataThe authors declare that no patient data appear in this article.
Right to privacy and informed consentThe authors declare that no patient data appear in this article.
Financial disclosureNo financial support was received in relation to this study/article.
Conflict of interestThe authors declare that there is no conflict of interest.
Please cite this article as: Martínez-Mier G, Esquivel-Torres S, Nava-Lacorte A, Lajud-Barquín FA, Zilli-Hernández S, Vázquez-Ramírez LM. Correlación de los niveles de alfafetoproteína sérica preoperatoria y sobrevida en el tratamiento quirúrgico del hepatocarcinoma en una unidad médica de alta especialidad en Veracruz, México. Revista de Gastroenterología de México. 2017;82:357–360.