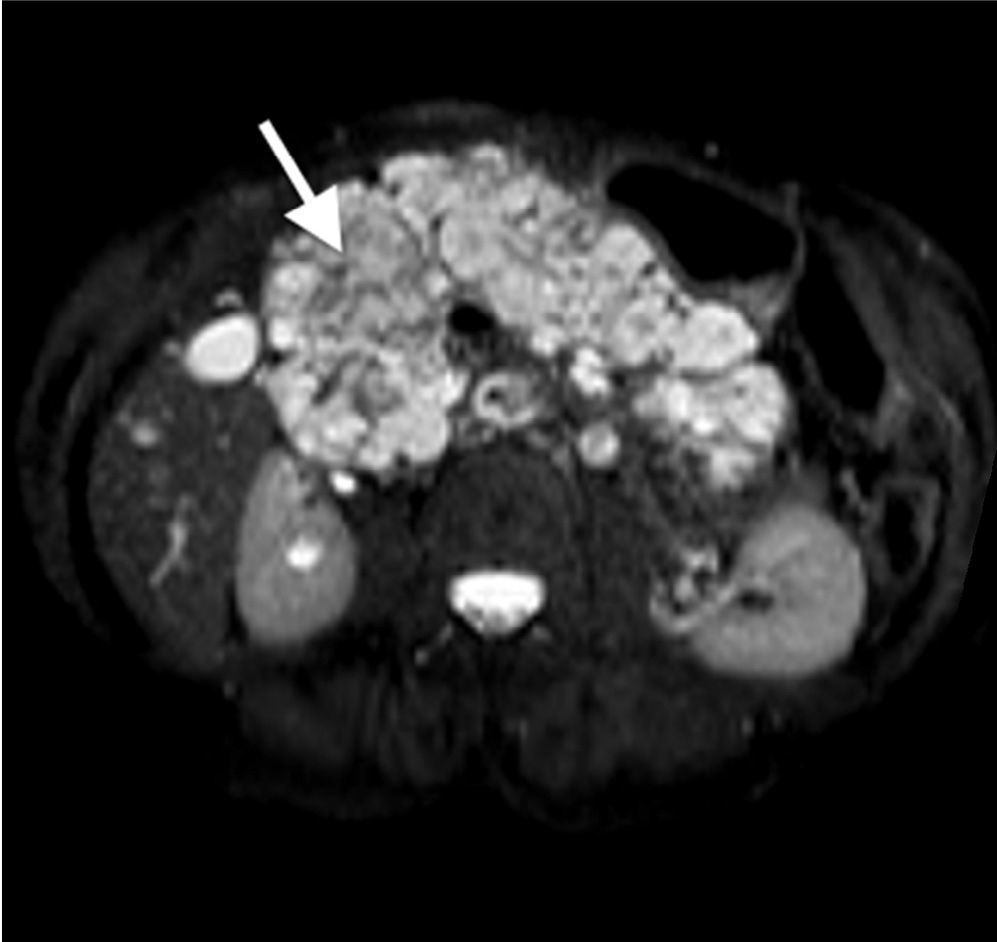
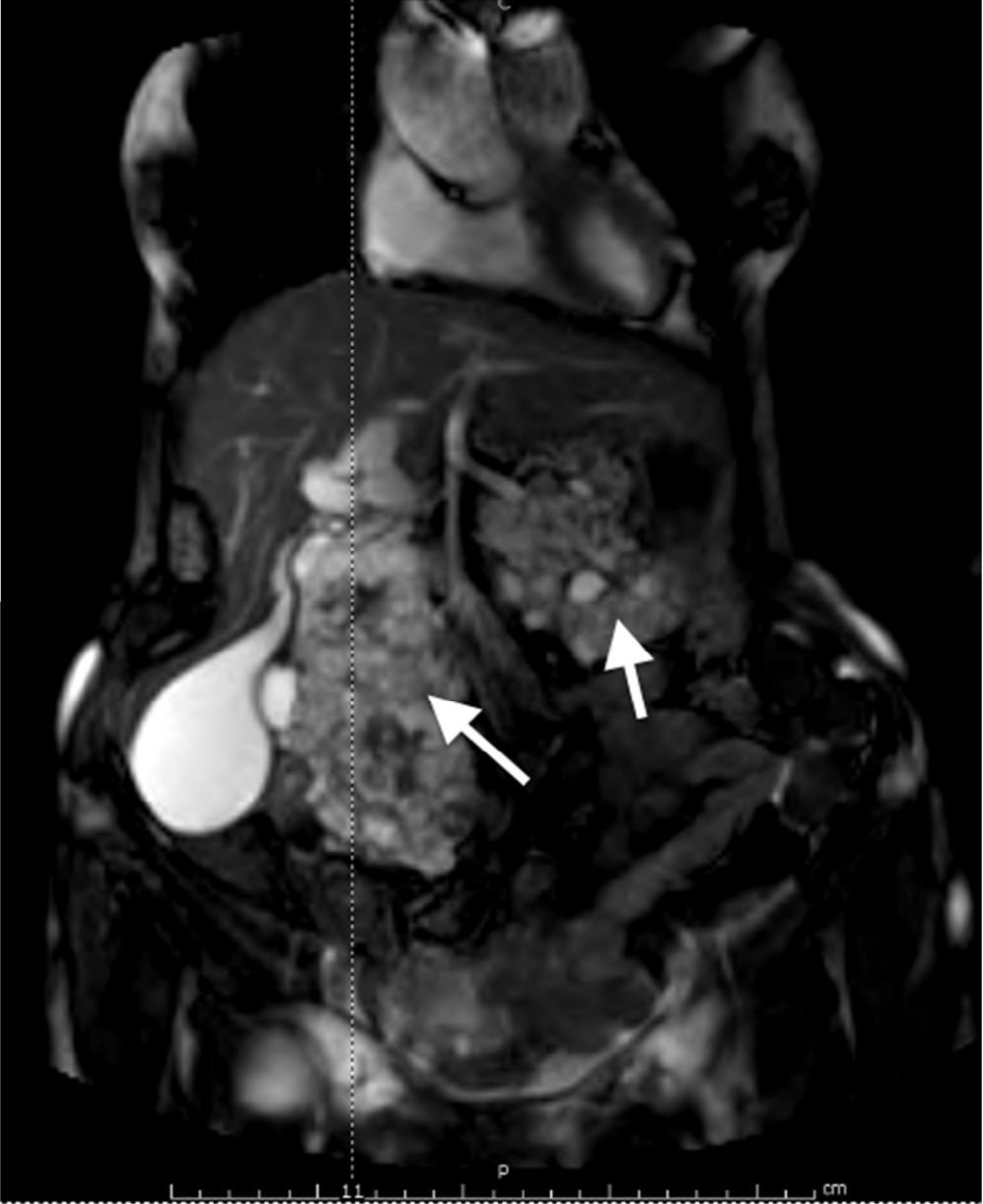
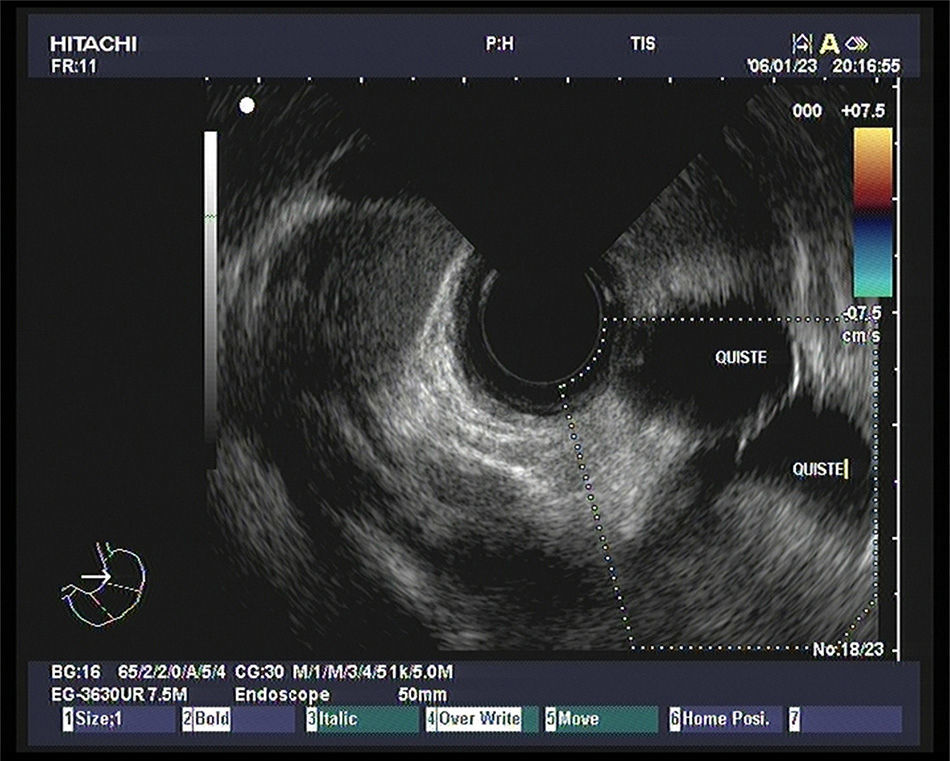
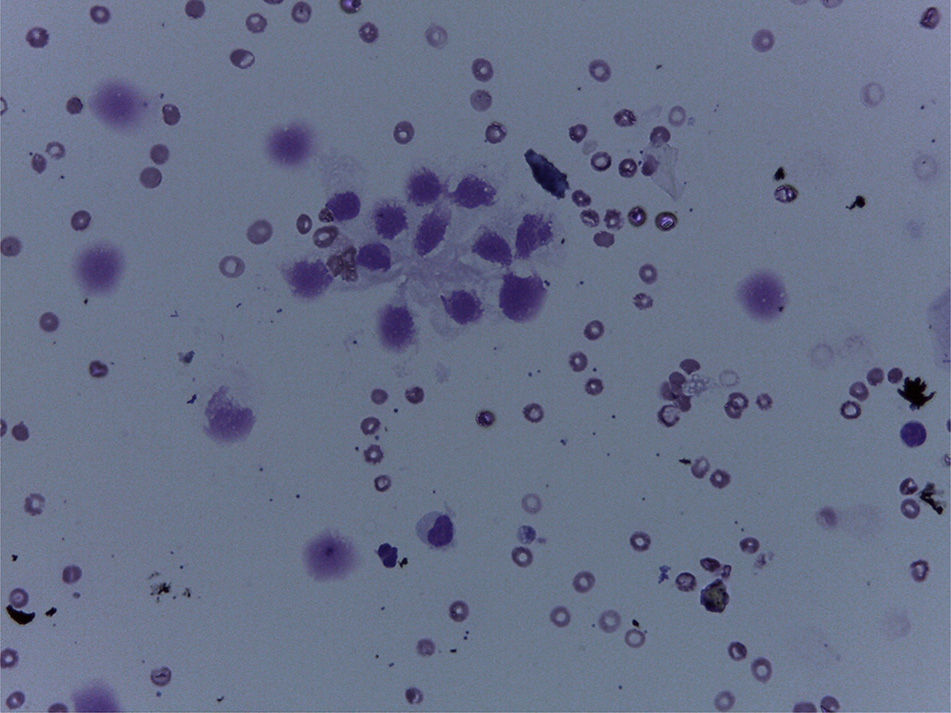
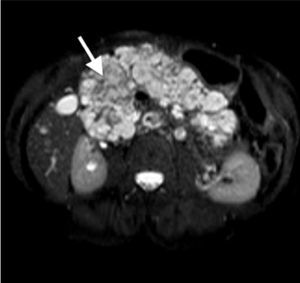
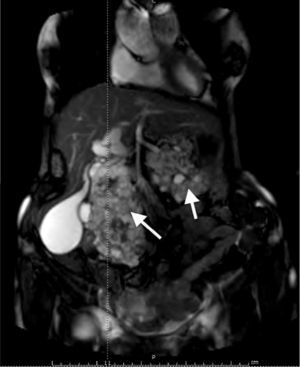
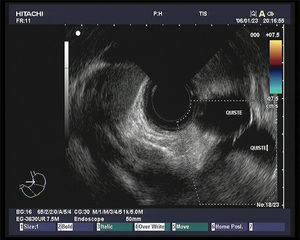
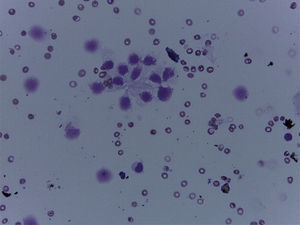
A 60-year-old woman with a history of cerebellar hemangioblastoma surgery and recently diagnosed diabetes mellitus sought medical attention for abdominal pain and a mass at the level of the epigastrium. Abdominal ultrasound revealed multiple pancreatic cysts. A consequently performed abdominal MR scan identified a strikingly enlarged pancreatic gland extending into the pelvis and multiple heterogeneous cystic lesions in its interior distributed in the head, body, and tail (Figs. 1 and 2). Echoendoscopic-guided FNA was performed (Fig. 3) and the cytology study was consistent with serous cystadenoma (Fig. 4). With the suspicion of von Hippel-Lindau syndrome, a genetic study was ordered that was positive for the 3p25-p26 mutation. During follow-up, endocrine pancreatic insufficiency progressed requiring insulin therapy and the patient developed diarrhea secondary to exocrine pancreatic insufficiency, needing enzyme supplements. The appearance of exocrine pancreatic insufficiency in von Hippel-Lindau disease is rare. In the present case, the important pancreatic involvement and its cystic transformation led to exocrine and endocrine insufficiency.
The same information as Figure 1.
The authors declare that no experiments were performed on humans or animals for this study.
Data confidentialityThe authors declare that no patient data appear in this article.
Right to privacy and informed consentThe authors declare that no patient data appear in this article.
Conflict of interestThe authors declare that there is no conflict of interest.
Please cite this article as: García García de Paredes A, Aguilera Castro L, Crespo Pérez L. Una causa infrecuente de epigastralgia. Revista de Gastroenterología de México. 2016;82:170–171.