We present herein the case of a 56-year-old man, with an unremarkable past medical history, who came to the emergency room complaining of abdominal pain of 3-day progression in the right hypochondrium. It began insidiously, with an intensity of 8/10, and was accompanied by abdominal bloating, hyporexia, and nausea. He did not present with vomiting, fever, or jaundice. The pain had no aggravating factors and partially improved with antispasmodics. Physical examination revealed reduced peristalsis, abdominal distension due to bloating, pain in the right hypochondrium upon palpation, and a positive Murphy’s sign.
The patient’s hemoglobin level was 12.4g/dl, platelets 336,000 cells/mm3, leukocytes 16,400 cells/mm3, and unaltered liver function tests. An upper abdominal ultrasound study identified a distended gallbladder with biliary sludge and a 3mm wall, a bile duct diameter of 5.5mm, and the remaining parameters within normal limits. Because the pain continued, a computed axial tomography (CAT) scan with intravenous contrast medium was carried out (Fig. 1). Whether the CAT images were caused by colonic pathology or by gallbladder pathology could not be accurately determined. Initial management was conservative, with bowel rest, analgesics, and double-regimen antibiotic therapy with ciprofloxacin and metronidazole for 7 days. The patient improved and was released under oral treatment with the same antibiotics for another 7 days. Six weeks later, a control CAT scan was performed that showed complete resolution of the perivesicular and pericolonic inflammation. The patient was asymptomatic at one month, then at 12 months, after his original symptoms.
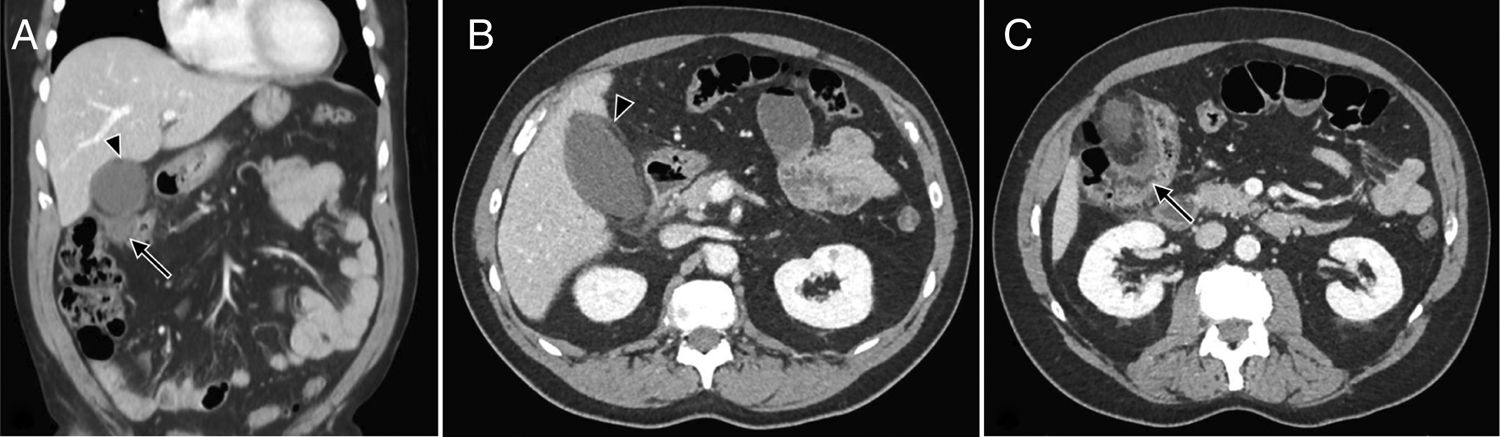
A. Coronal view, the presence of pericholecystic inflammatory changes (arrowhead) and a pericolonic phlegmon (arrow), B. Axial view, perivesicular inflammatory changes, fat stranding at that level, data that could suggest acute cholecystitis, C. Axial view, thickening of the colonic wall of the hepatic flexure and pericolonic fat stranding, with active diverticular disease.
The present case is a rare variant of diverticular disease, given that the most commonly affected site is the sigmoid colon in white patients and the right colon in Asians.1 Three main factors are known to cause diverticular disease: disordered intestinal motility, a low-fiber diet, and intestinal wall abnormalities.2
Diverticular disease in the transverse colon or hepatic flexure, first described in 1944 by Thompson and Fox, is extremely infrequent.3 It accounts for only 5 to 10% of all diverticulitis in the large intestine. Inflammation or perforation of the diverticula in that zone is very rare, occurring in only 0.5-2.7% of cases.4 The most commonly related presumptive diagnosis in patients with diverticular disease of the right colon is acute appendicitis, with some published case reports.5 Even less frequent is a clinical picture similar to that of acute cholecystitis secondary to diverticulitis of the right colon or transverse colon, as in our patient, and we know of the report of only one such case.4 To confirm the diagnosis, computed tomography must show thickening of the colonic wall and an increase in the density or stranding of the pericolonic fat, as well as possible pericolonic abscesses and intramural and extraluminal air.6 The first 3 characteristics were observed in the CAT scan of our patient, which, added to the intramural air, resulted in the definitive diagnosis. Some studies indicate that diverticulitis of the right colon is more benign than that of the left colon. Surgical management is extremely rare and antibiotic therapy is the treatment of choice in such cases.7 Successful management has even been reported with bowel rest and hydration, with no need for antibiotic therapy.8 The majority of patients that have an episode of acute diverticulitis will not have a new episode throughout their lifetime and only around 20% of patients will have disease recurrence at 5 years.9 Specifically in diverticulitis of the right colon, Wegdam et al. reported 7% recurrence at 7 years of follow-up.7 Our patient recovered completely with conservative treatment, and at the time of writing this report, has not had a relapse of the disease.
The clinical diagnosis of acute diverticulitis is a challenge in cases such as the one presented herein. Even though it is uncommon, our case shows the importance of considering diverticulitis of the right colon or the transverse colon in the differential diagnoses for acute cholecystitis. In patients that present with abdominal pain in the right upper quadrant, but with symptoms that do not concur with hepatobiliary pathology, CAT imaging can be the first-line study for making the diagnosis. Likewise, that imaging method is very capable of showing the segmental thickness of the intestinal wall, stricture zones, and the complications of fistulas and abscesses. In addition, it possesses multi-plane reconstruction algorithms that enable better evaluation of the anatomic changes of the gastrointestinal tract and other abdominal organs.10
Finally, it is important to emphasize the adequate response to conservative management that has presented in other cases, as in our patient, preventing the morbidity and mortality of surgical management.
Ethical disclosuresProtection of human and animal subjects. The authors declare that no experiments were performed on humans or animals for this study.
Confidentiality of data. The authors declare that they have treated all patient data with confidentiality and anonymity, following the protocols of their work center.
Right to privacy and informed consent. The authors declare that no patient data appear in this article.
Right to privacy and informed consent. The authors have obtained the written informed consent of the patients or subjects mentioned in the article. The corresponding author is in possession of this document.
Financial disclosureNo specific grants were received from public sector agencies, the business sector, or non-profit organizations in relation to this study.
Conflict of interestThe authors declare that there is no conflict of interest.
Please cite this article as: Gonzalez-Urquijo M, Baca-Arzaga A, Lozano-Balderas G. Diverticulitis aguda del ángulo hepático simulando un cuadro de colecistitis aguda. Revista de Gastroenterología de México. 2020;85:484–486.