Gangliocytic paraganglioma (GP) is a rare gastrointestinal tumor and 90% of the cases are found in the duodenum, with a predilection for the region of the ampulla of Vater.1–3 The most common clinical presentation includes melena and abdominal pain and it typically follows a benign course.1–3 Surgical resection is the most common treatment and only around 20 cases managed with endoscopic resection have been reported. Up to now, endoscopic resection has shown lower morbidity and mortality, compared with local surgical excision.1,4
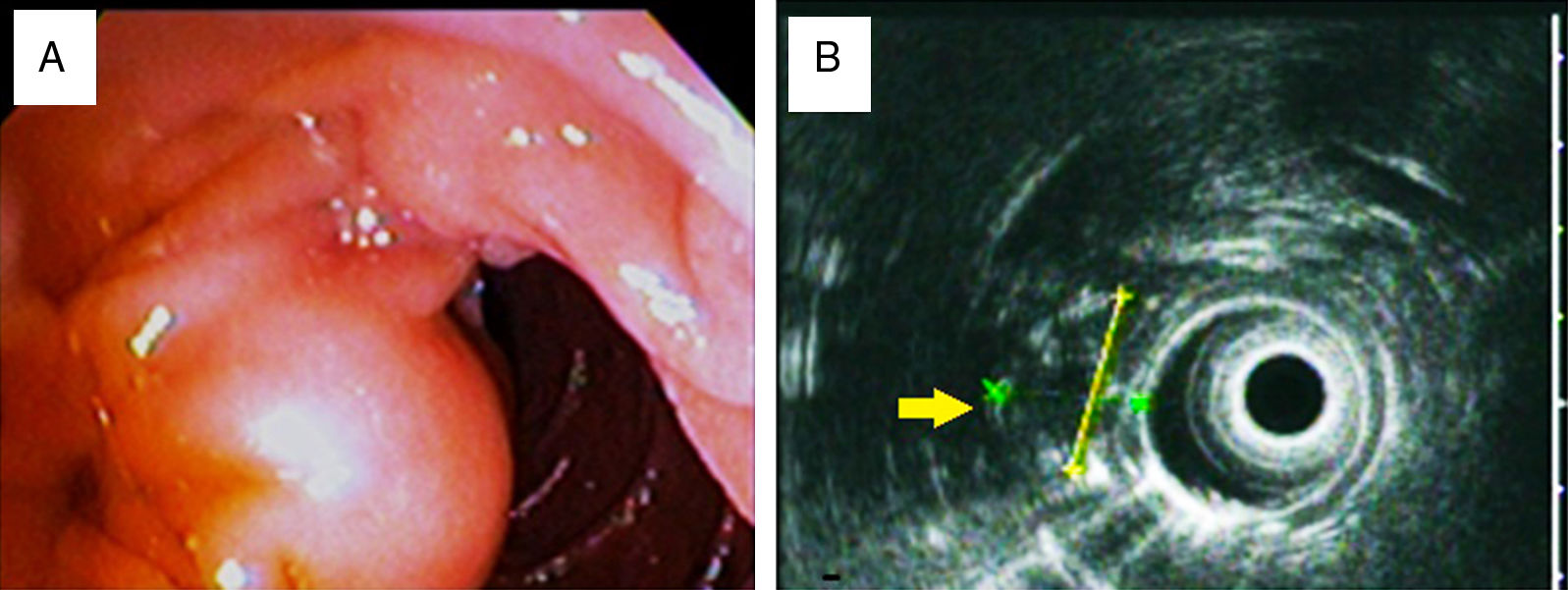
We present herein the case of a 65-year-old woman who sought medical attention for symptoms of one-year progression that included intermittent nausea, occasional epigastric pain, and involuntary weight loss of 12kg. Physical examination and laboratory work-up revealed no relevant pathologic data. Panendoscopy was performed showing images of a subepithelial ampullary lesion (fig. 1) and endoscopic ultrasound identified a submucosal tumor 21mm in diameter adjacent to the ampulla of Vater that did not affect the muscular layer of the duodenum. There were no local adenopathies (fig. 1). An abdominal tomography scan showed no evidence of lymph node or vascular invasion.
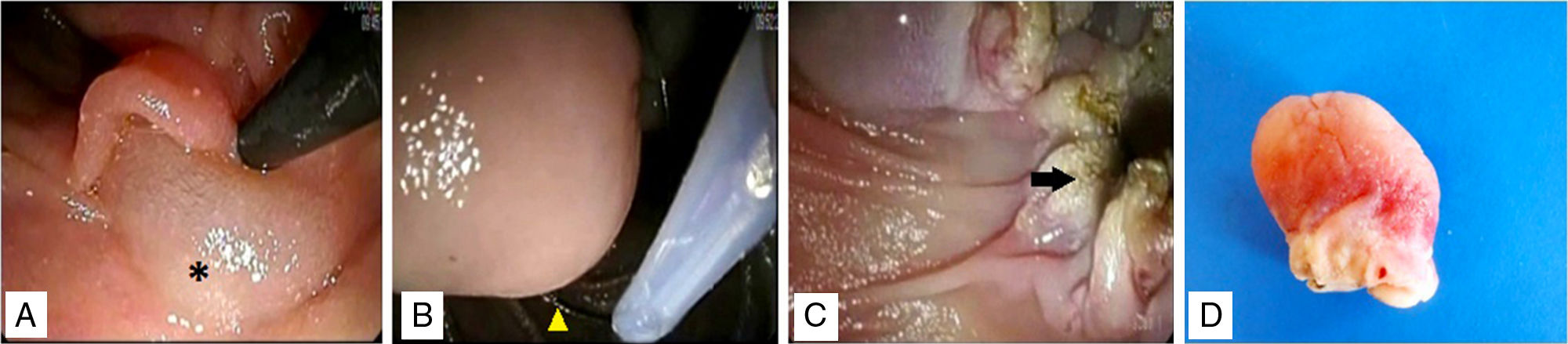
Endoscopic ampullectomy was performed (fig. 2), completely resecting the lesion and following the standards proposed in the international guidelines,5 except for the placing of a pancreatic stent, because cannulation of the papilla was impossible. The patient presented with mild acute pancreatitis that resolved satisfactorily with conservative medical therapy, and so she was released from the hospital on day 5 after the endoscopic procedure. The histopathologic study and immunolabeling of the surgical specimen reported GP with lesion-free edges. A positron emission tomography scan and new duodenoscopies at 6, 12, 18, and 24 months were carried out as part of the follow-up and they showed no signs of recurrence.
Endoscopic papillectomy. A) Infiltration of the base of the lesion with 0.9% saline solution with epinephrine, showing the “lifting” phenomenon (asterisk). B) Polypectomy loop placement (arrowhead) “lassoing” the lesion from its base. C) Complete resection of the lesion. Edges with no signs of bleeding in the duodenal wall (arrow). D) Surgical specimen.
GP was first described in 1957 by Dahl, as a “duodenal ganglioneuroma”,6 and only around 200 cases have been reported to date.7
Endoscopically, the majority of gangliocytic paragangliomas are described as an elevated, submucosal lesion with well-defined edges. In some cases, pedicles and ulcerations can be observed.1,4
The most important diagnostic quality is a typical triphasic histologic pattern that includes a mixture of lymph node cells, areas similar to a carcinoid tumor, and a proliferation of spindle cells.2 In the present case, in addition to observing this histologic characteristic, immunohistochemical staining was carried out for synaptophysin, S-100 protein, and neurofilaments, thus concluding the GP diagnosis.
Only approximately 5-7% of duodenal GPs metastasize to regional lymph nodes and invade neighboring structures.7 Recurrence is rare and generally occurs 11 years after the initial resection.4,7,8 In 2014, Li et al.8 reported a case of GP of malignant duodenal origin with multiple distant metastases and a lethal course. Pancreaticoduodenectomy with lymph node dissection has thus been suggested as ideal treatment,8 but it is associated with a high rate of perioperative mortality (approximately 4%) and complications such as biliary leakage or delayed gastric emptying.2,4,8 Given the abovementioned and the fact that most GPs are benign, local surgical excision or endoscopic resection is sufficient.
The American Society for Gastrointestinal Endoscopy (ASGE) has proposed the following criteria for endoscopic resection of ampullary lesions:51) a size smaller than 4-5cm, 2) no macroscopic evidence of malignancy, 3) benign histology, and 4) absence of ductal invasion or invasion that is under 1cm. In the present case, the GP had the necessary characteristics for a safe endoscopic resection. First, submucosal infiltration was carried out until achieving the “lifting” of the lesion using the “snare technique” (the technique that our unit has the most experience with), which helps reduce the risk for bowel perforation. Papillectomy was then successfully performed. It should be mentioned that there is still no internationally well-established and totally accepted resection technique or criteria.
Adverse events resulting from the endoscopic resection of ampullary lesions present in approximately 10% of cases,5 and they include pancreatitis, perforation, bleeding, cholangitis, and others associated with sedation. Mild-to-moderate pancreatitis is the most frequent complication,5 and in the case of our patient, remitted after 72h. Most likely it appeared due to the inability to place a pancreatic stent, even though there are no clinical trials showing that such placement reduces the risk for developing pancreatitis.
The present case of GP successfully managed through endoscopy is the first to be reported in Mexico. Other Mexican authors9,10 have described similar GPs, but the approach was surgical, and even though they reported no immediate complications, hospital stay was 7 days, increasing the cost of that treatment modality, compared with endoscopy.
With our report, we hope to motivate new related studies, offering patients an efficacious treatment that is both less costly and less invasive.
Conflict of interestThe authors declare that there is no conflict of interest.
Please cite this article as: Palomino-Martínez BD, Espino-Cortés H, Cerna-Cardona J, Godínez-Martínez LE, Chávez-García MA. Paraganglioma gangliocítico duodenal. Tratamiento mediante resección endoscópica. Revista de Gastroenterología de México. 2018;83:198–199.