Achalasia is the most widely studied esophageal motility disorder. No treatment has achieved completely satisfactory results. The laparoscopic Heller esophagomyotomy is currently the most accepted technique. With the advent of minimally invasive surgery, the appearance of peroral endoscopic myotomy (POEM) has promising results. The primary aim of our study was to perform peroral endoscopic esophagomyotomy in animal experimentation models to perfect the technique and later apply it to humans. The secondary aims were to evaluate the intraoperative and postoperative complications and to describe the anatomopathologic findings.
Materials and methodsAn experimental study was conducted on 8 live porcine models that were followed for 30 days to identify postoperative complications. Necropsy was then performed to evaluate the histopathologic findings. The international requirements and regulations for animal experimentation were met.
ResultsThe technique was carried out in all the models. There was one intraoperative death. Pneumothorax was observed in 50% of the units in experimentation and subcutaneous cervical emphysema in 75%, with no significant clinical repercussions. Histologic muscle layer (myotomy) involvement was above the gastroesophageal junction in 87% of the cases and below it in 25%.
ConclusionPeroral endoscopic esophagomyotomy is a feasible, albeit complex, procedure that requires advanced training, and thus should be performed in highly specialized centers. Specific skills in advanced therapeutic endoscopic procedures of this type must continue to be developed through continuing education (ideally in in vivo models), to then be performed on humans.
La acalasia es el trastorno de motilidad esofágica más estudiado; ningún tratamiento ha logrado resultados completamente satisfactorios. La esofagomiotomía de Heller por laparoscopia es la técnica más aceptada en la actualidad. Con el advenimiento de la cirugía mínimamente invasiva, aparece la miotomía endoscópica submucosa con resultados prometedores. Nuestro objetivo principal de este estudio fue realizar miotomía endoscópica submucosa en modelos de experimentación animal, para perfeccionar la técnica y posteriormente aplicarla en humanos. Como objetivo secundario se buscó evaluar las complicaciones intra y postoperatorias, así como describir los hallazgos anatomopatológicos encontrados.
Materiales y métodosSe realizó un estudio experimental en 8 modelos porcinos vivos, que se siguieron durante 30 días para identificar complicaciones posoperatorias. Posteriormente se practicó necropsia evaluando los hallazgos histopatológicos. Se cumplieron los requisitos y regulaciones internacionales de experimentación en animales.
ResultadosSe logró realizar la técnica en todos los modelos. Se presentó una mortalidad intraperatoria. Se observó neumotórax en el 50% y enfisema subcutáneo en el 75% de las unidades de experimentación, sin repercusión clínica significativa. Se observó compromiso histológico de la capa muscular (miotomía) por encima de la unión esofagogástrica en el 87% de los casos y por debajo de esta en el 25% de los casos.
ConclusiónLa esofagomiotomía endoscópica submucosa es un procedimiento factible pero complejo que requiere un entrenamiento avanzado, y dadas sus características debe ser realizado en centros de alta complejidad. Es necesario seguir desarrollando destrezas específicas, mediante educación continuada (idealmente en modelos in vivo), en procedimientos endoscópicos terapéuticos avanzados de este tipo, para posteriormente ser desarrollados en humanos.
Achalasia is the best-described esophageal motility disorder. It is a disease of unknown pathophysiology that significantly compromises patient quality of life, for which there is no curative treatment.1 Laparoscopic Heller myotomy associated with partial fundoplication is the surgical treatment of choice, even though there are some alternatives that offer similar results, such as endoscopic pneumatic balloon dilation.2,3 The technique of endoscopic botulinum toxin injection, widely used in patients that are not candidates for surgical management, has limitations regarding costs and the need for numerous procedures, as well as varying results. The development of therapeutic endoscopy and the ever-increasing knowledge about the deep layers of the gastrointestinal tract, has made the concept of natural orifice translumenal endoscopic surgery possible.4 This is how peroral endoscopic esophagomyotomy (POEM) emerged as a management alternative, demonstrating similar, and even superior, results to the current techniques.5,6
POEM has been evaluated in pigs and in humans. The potential benefits of this technique are less postoperative pain, reduced incision-derived complications, shorter hospital stay, and better cosmetic results.3,6 Endoscopic submucosal dissection (ESD) is the basic technique for the development of POEM.7,8 In Colombia, experience with ESD has been reported on,7,8 but up to now, no experience with POEM has been published in either animal or human experimental models.
The use of in vivo experimental models is important in the research on and development of special medical surgical techniques. The purpose of this type of work is to improve skills and gain experience in the performance of POEM, in the hope of establishing it as the management of choice for achalasia.9,10
The primary aim of our study was to perform POEM on animal experimentation models to perfect the technique and later perform it on humans. The secondary aims were to evaluate the intraoperative and postoperative complications and to describe the anatomopathologic findings.
Materials and methodsAn experimental study on animal models (pigs) was conducted for the performance of POEM. Eight endoscopic surgeries were carried out under general anesthesia administered by a veterinarian. All the procedures were performed by the same surgeon with vast experience in therapeutic endoscopy (more than 10 years). His interventions include 2,000 biliary tract operations (endoscopic retrograde cholangiopancreatography) and numerous ESD procedures, the latter technique learned in formal courses (IRCAD-University of Strasbourg-France) under the supervision of Asian experts.7–19 The 8 pigs utilized were of the same race and had similar weights and ages. The POEM technique parameters described by Inoue11were followed. The esophagogastric junction was located and a submucosal injection of 0.9% saline solution was applied 10cm above it. A 2cm longitudinal incision was made, beginning the creation of a submucosal tunnel utilizing Fujifilm EG-530WR® endoscopic video equipment, a Fujifilm 4450-HD® processor, a Triangle Tip–Knife® endoscopic scalpel (Olympus Medical Systems®), and an ERBE VIO 200 S® electrosurgical unit. All the procedures were carried out under CO2 insufflation with Fujifilm GW-1® equipment. The tunnel was extended up to approximately 3cm under the esophagogastric junction. Myotomy was then performed, involving the circular muscle layer, 8cm cranial to 2cm caudal from the esophagogastric junction. The mucosa was closed with KDL-135® endoscopic clips (Olympus Medical Systems®).
The intraoperative variables were evaluated, and a 30-day follow-up of the experimental units was carried out to identify complications and mortality. The experimental model follow-up included tolerance of oral diet or the appearance of inflammatory response symptoms. On day 30 of the follow-up, the veterinarian euthanized the animals to evaluate the macroscopic and microscopic pathologic variables and identify complications, such as mediastinitis, peritonitis, and abscesses. In addition, the histologic involvement of the esophageal layers was evaluated to test the myotomy. Five histologic cuts were made in the pathologic specimen: at 9cm (cut 1), 4cm (cut 2), and 1cm (cut 3) above the esophagogastric junction; and at 2cm (cut 4), and 4cm (cut 5) below the esophagogastric junction. Hematoxylin-eosin stain was used for the histologic evaluation. The special Masson's trichrome stain was applied to 3 specimens for improved test performance10 and to verify the histologic involvement of the muscle layer. The data were entered into the Excel 2010 program and later tabulated using the STATA version 12 software.
Ethical considerationsThe present study was conducted following the regulations stipulated in the 1989 Law 84 and those annotated in Article 87 of the 1993 Resolution number 8430 of the Republic of Colombia. They include the legal acquisition of animals and the use of the minimum number of experimental units. The animals were treated as sensitive mammals during the procedures to ensure their well-being and prevent pain. Finally, they were euthanized with no suffering. Complying with the requisites for experimental model use, the study was approved by the Ethics Committee of the CICUAL de Anestol SAS on animal use in experimentation, as well as by the Ethics Committee of the Research Division of the University Health Sciences Foundation.
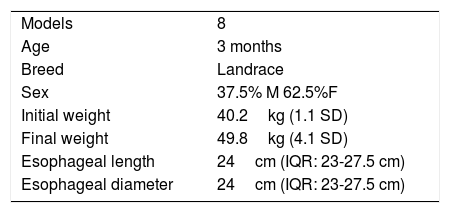
ResultsA total of 8 endoscopic procedures were performed on animal experimentation models (3-month old Landrace pigs, 5 males and 3 females). The mean initial weight of the pigs was 40kg (1.1 SD) and it was 49.8kg (4.1 SD) at the end of the 30-day follow-up. Overall mortality was 12.5% and all deaths occurred intraoperatively. The median surgery duration was 147min (IQR: 115-182) and the median anesthesia duration was 186min (IQR: 152.2-225.5) (Table 1).
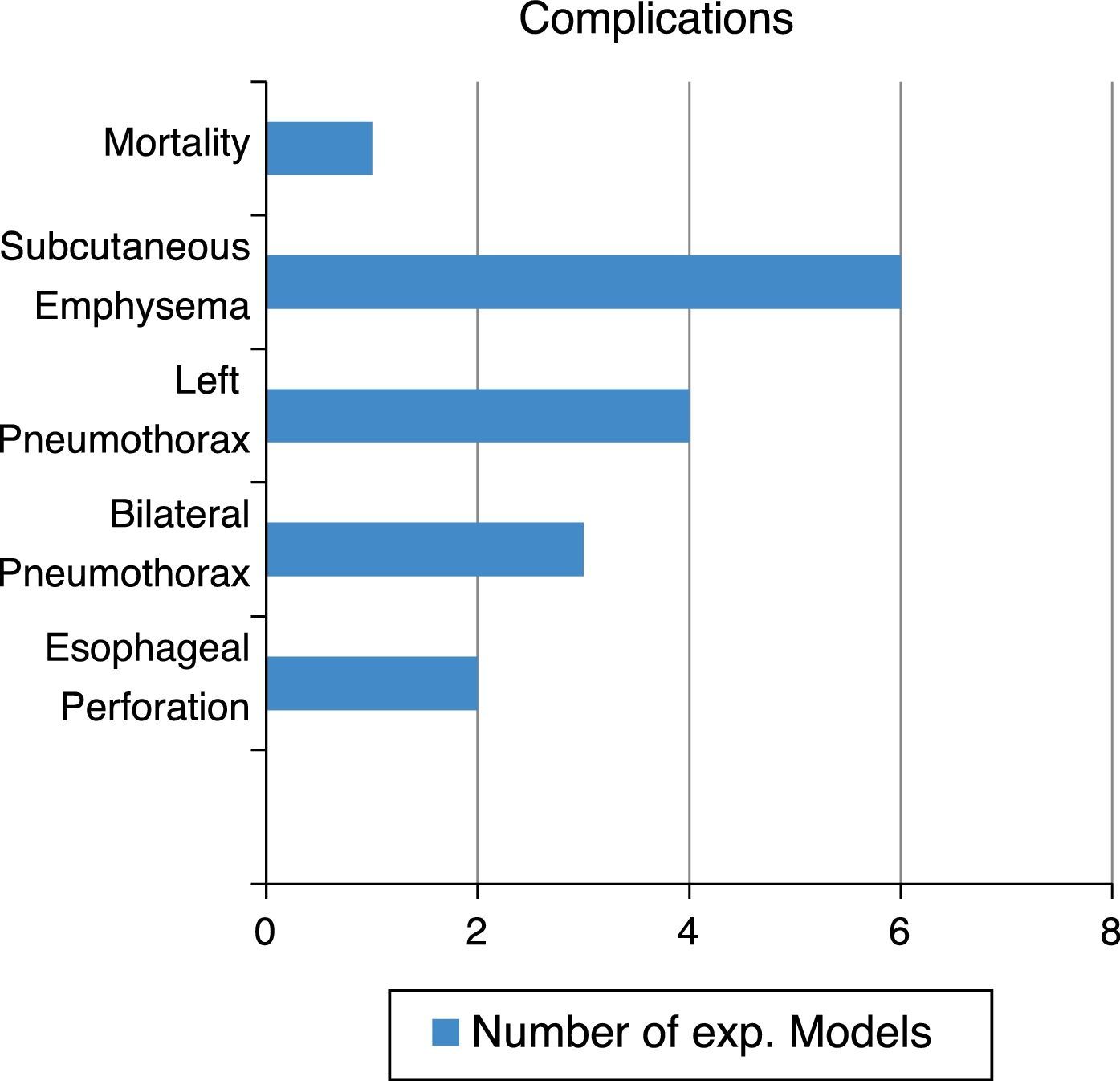
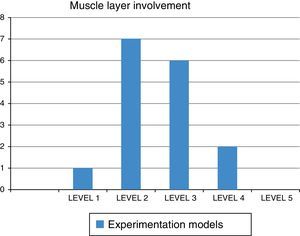
A mean of 13.5 clips was employed for closure of the mucosa (5.75 SD). Intraoperative esophageal perforation was observed in 12.5% of the models and the intraluminal mucosa was closed in one of them during the creation of the submucosal tunnel. Fifty percent of the animals presented with left pneumothorax and 37.5% with bilateral pneumothorax that was successfully managed with underwater seal chest drains. Subcutaneous cervical emphysema was observed in 75% of the models. Only one of the models presented with postoperative fever during the first 48h and adequate response was achieved through antibiotic management. No other complications were observed in the follow-up of the other animals (fig. 1).
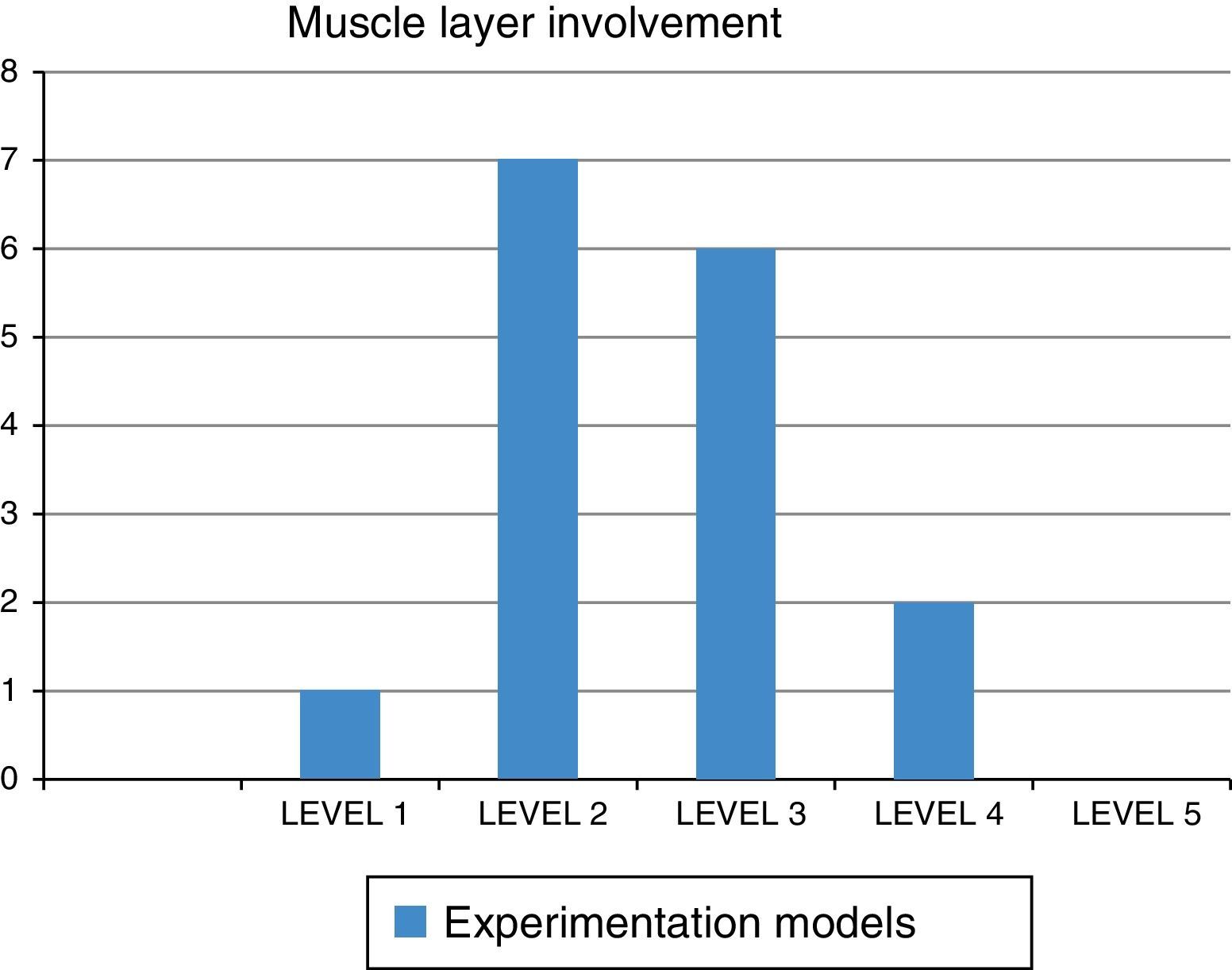
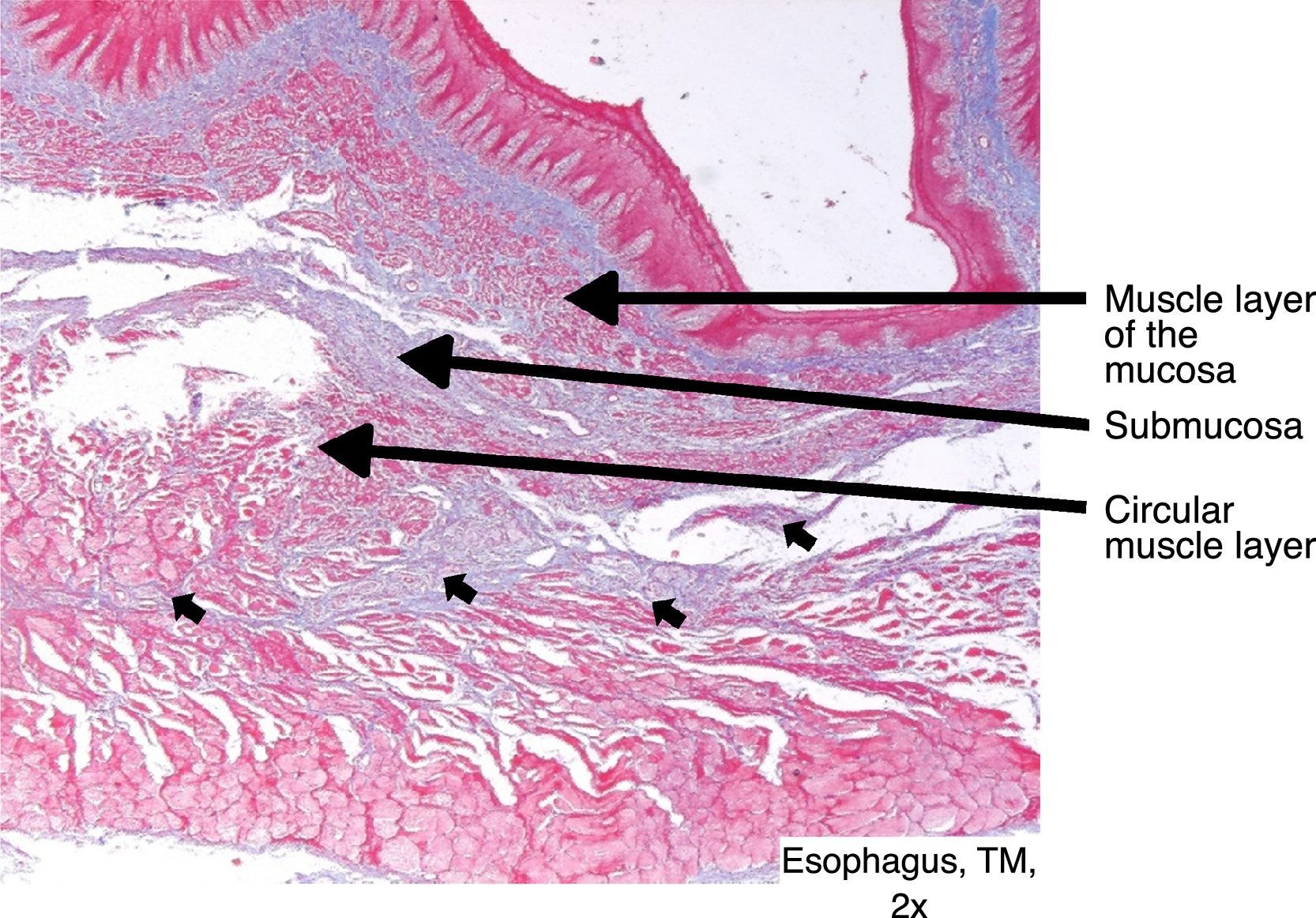
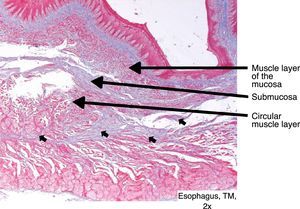
Regarding the pathologic findings, there were no macroscopic signs of complications (mediastinitis, peritonitis, etc.), except the intraoperative perforation identified in the first model. Median esophageal length was 24cm (IQR: 23-27.5) and median esophageal diameter was 1.5cm (IQR: 1.35-1.65cm). There was histologic involvement of the muscle layer in esophageal cuts number 1 (12.5%), number 2 (87.5%), number 3 (75%), and number 4 (25%). No muscle involvement was observed in any cut number 5 (4cm distal from the cardioesophageal junction). There was involvement of the serosa layer (microscopic perforation) in 2 models. In one, the finding was intraoperative and in the other it was microscopic (12.5%) (figs. 2 and 3).
Discussion and conclusionsThe results of our study on pig models were similar to those reported in other countries,12 which is of great importance in our medical environment. The intraoperative mortality that presented in experimentation model number 1 was secondary to a perforation in the esophageal serosa, compromising the pleura, despite underwater seal chest drain management. The mean duration of the procedure was very close to that reported in Asian countries for this technique in humans (120minutes).6 More clips were used for closure of the mucosa (a mean of 8) than the quantity described in procedures on humans,13 which we consider secondary to the required learning curve for said closure. The majority of the porcine experimentation models presented with pneumothorax, but there was only one macroscopic perforation that compromised the pleura. Subcutaneous cervical emphysema was observed in the majority of the pigs, which has also been reported in previous animal studies.9,10 Even though we observed no macroscopic perforations in those cases, we believe the emphysema corresponded to diffusion of the CO2 employed, because immediately after the procedure ended, the emphysema disappeared, and no microperforations were found in the pathology study of the majority of the models. However, this last possibility cannot be completely ruled out, given the distance between the histologic cuts. The pathology studies reported no infectious complications (mediastinitis, peritonitis, para-esophageal abscesses, etc.) in any of the models. One of the pigs presented with fever but did not meet the criteria for hemoculture or sacrifice, according to the study protocol. The histologic sections demonstrated muscle layer involvement above the esophagogastric junction in the majority of the experimentation models, but minimal compromise in the sections from 2cm and 4cm below the esophagogastric junction, indicating that the aim of the myotomy was not achieved. The amount of experience of the gastroenterologist with this procedure, the reduced thickness of the muscle layer in the pig, and the absence of hypertrophy found in true achalasia most likely contributed to those results. This does not imply that the POEM procedure is less clinically effective in human patients that actually present with achalasia, given that other endoscopic techniques (pneumatic dilation) do not involve those fibers and the results are similar.2 The development of experimental studies on live animals represents a great economic and academic investment, but we consider it an essential part of biomedical research.14
The limitations of our study include the reduced number of animal experimentation models, demanded by the ethical norm (minimal number of experimentation units).14 In addition, it was not possible to perform preoperative and postoperative esophageal manometry, which would have enabled the difference of lower esophageal sphincter pressure, before and after the procedure, to be analyzed.15 This could not be done, because of the unavailability in Colombia of animal digestive physiology equipment. We attempted to verify the effectiveness of esophagomyotomy through sequential histologic sections, but it was not possible to differentiate the muscle involvement between the circular and longitudinal layers, due to the inflammatory and regeneration processes (characteristic of survival experiments). However, it should be noted that the muscle layer section was verified in the zone of clinical interest in the majority of the models. Finally, it must be remembered that pigs do not present with achalasia and the muscle layer is significantly thinner than that in humans, mainly in the caudal region. Additionally, the adventitia is practically adhered to the pleura at that level, according to veterinary studies.16 All the above, makes it difficult to equate the results of studies conducted on pigs with those on patients with achalasia. According to the study protocol, the pathology results were obtained at the end of the study, and therefore it was not possible to make decisions during the study that would have improved its effectiveness (e.g. length and depth of the myotomy).
Despite those limitations, the use of porcine models is the most suitable method for developing the POEM technique,9 and to the best of our knowledge, the present study is the first South American article on this topic to be published.
Our results suggest that endoscopic esophagomyotomy is a procedure requiring significant training and development of skills on animal experimentation models, for later performance on humans. This should ideally be carried out in a research protocol that has university support and is performed in advanced speciality medical centers. It is necessary to continue to develop specific skills in these types of advanced therapeutic endoscopy procedures (natural orifice translumenal endoscopic surgery, ESD, POEM, etc.) through continuing education, because they have a long learning curve. In relation to POEM, the learning curve can require up to 50 procedures in humans.18,19
Ethical disclosuresProtection of human and animal subjectsThe authors declare that the procedures followed were in accordance with the regulations of the relevant clinical research ethics committee and with those of the Code of Ethics of the World Medical Association (Declaration of Helsinki).
Confidentiality of dataThe authors declare that they have followed the protocols of their work center on the publication of patient data.
Right to privacy and informed consentThe authors declare that no patient data appear in this article.
Financial disclosureThis study was completely funded by the Research Division of the University Health Sciences Foundation of the Hospital San José, Bogotá.
Conflict of interestBecause the present study was an academic protocol, the financial support from the Research Division of the University Health Sciences Foundation does not create a conflict of interest.
Please cite this article as: Peñaloza-Ramírez A, Suárez-Correa J, Báez-Blanco J, Sabogal-Gómez C, Kuan-Casas H, Sánchez-Pignalosa C, et al. Miotomía endoscópica peroral, experiencia in vivo: imprescindible para desarrollo de la técnica en humanos. Revista de Gastroenterología de México. 2018;83:86–90.