The prevalence of Barrett's esophagus has been calculated at between 1.3 and 1.6%. There is little information with respect to this in Mexico.
AimTo determine the frequency and characteristics of Barrett's esophagus in patients that underwent endoscopy at a national referral center, within a 10-year time frame.
Material and methodsThe databases of the pathology and gastrointestinal endoscopy departments of the Instituto Nacional de Ciencias Médicas y Nutrición “Salvador Zubirán” were analyzed, covering the period of January 2002 to December 2012. Patients with a histologic diagnosis of Barrett's esophagus were included. The variables of age, sex, the presence of dysplasia/esophageal adenocarcinoma, Barrett's esophagus length, and follow-up were analyzed.
ResultsOf 43,639 upper gastrointestinal endoscopies performed, 420 revealed Barrett's esophagus, corresponding to a frequency of 9.6 patients for every 1,000 endoscopies. Of those patients, 66.9% (n=281) were men, mean patient age±SD was 57.2±15.3 years, 223 patients (53%) presented with long-segment Barrett's esophagus, and 197 (47%) with short-segment Barrett's esophagus. Dysplasia was not present in 339 patients (80.7%). Eighty-one (19.3%) patients had some grade of dysplasia or cancer: 48/420 (11.42%) presented with low-grade dysplasia, 20/420 (4.76%) with high-grade dysplasia, and 13/420 (3.1%) were diagnosed with esophageal cancer arising from Barrett's esophagus. Mean follow-up time was 5.6 years.
ConclusionsThe frequency of Barrett's esophagus was 9.6 cases for every 1,000 upper gastrointestinal endoscopies performed. Dysplasia was not documented in the majority of the patients with Barrett's esophagus and they had no histopathologic changes during follow-up. A total of 19.3% of the patients presented with dysplasia or cancer.
La prevalencia de esófago de Barrett (EB) se ha calculado entre el 1.3 y el 1.6%. En México existen pocos datos al respecto.
ObjetivoDeterminar la frecuencia y características del EB en pacientes sometidos a endoscopia en un centro de referencia nacional, en un periodo de 10 años.
Material y métodosSe analizaron bases de datos de los departamentos de Patología y Endoscopia Gastrointestinal del Instituto Nacional de Ciencias Médicas y Nutrición «Salvador Zubirán» (INCMNSZ), en el periodo comprendido de enero del 2002 a diciembre del 2012. Se incluyó a pacientes con diagnóstico histológico de EB. Se analizaron edad, sexo, presencia de displasia/adenocarcinoma de esófago, longitud del EB y seguimiento.
ResultadosSe realizaron 43,639 endoscopias de tubo digestivo superior, se incluyó a 420 pacientes con EB, lo que corresponde a una frecuencia de 9.6 pacientes por cada 1,000 estudios realizados. El 66.9% (n = 281) fueron hombres; la edad media±DE fue de 57.2±15.3 años; 223 pacientes (53%) presentaron EB de segmento largo y 197(47%) de segmento corto; 339 pacientes (80.7%) no presentaron displasia, 81(19.3%) tuvieron algún grado de displasia o cáncer; de estos, 48/420 (11.42%) displasia de bajo grado, 20/420 (4.76%) displasia de alto grado y 13/420 (3.1%) tuvieron el diagnóstico de cáncer esofágico originado en EB. El seguimiento promedio fue de 5.6 años.
ConclusionesLa frecuencia de EB fue de 9.6 casos por cada 1,000 endoscopias de tubo digestivo superior. En la mayoría de los pacientes con EB no se documentó displasia y permanecieron sin cambios histopatológicos durante el seguimiento. El 19.3% de los pacientes presentaron displasia o cáncer.
Barrett's esophagus (BE) is defined as the replacement of the squamous epithelium of the distal portion of the esophagus with columnar epithelium, suspected at endoscopy and corroborated through histopathology.1 It is significant because it is a premalignant lesion and is considered the most important risk factor for developing esophageal adenocarcinoma. Patients with BE have a 30 to 125-fold greater risk for presenting with esophageal adenocarcinoma, compared with individuals with normal epithelium.2 Its prevalence in population studies has been calculated at between 1.3 and 1.6%,3–5 and the annual incidence of esophageal adenocarcinoma in those populations is 0.26 to 0.38%.2,6,7 A study conducted in Mexico in 20058 analyzed 4,947 endoscopic studies over a 3-year period and detected a total of 13 cases of BE (a frequency of 0.26%). That same year another study was published on patients with typical gastroesophageal reflux disease (GERD) symptoms corroborated through the Carlsson-Dent questionnaire. The study included 109 patients that consecutively underwent endoscopy and BE was found in 10 patients (prevalence of 9.6%).9 Since then, no studies on this pathology have been published in Mexico. The follow-up of Mexican patients diagnosed with BE is carried out in accordance with international guidelines based on data from populations in the United States and Europe.1,10,11 There are Mexican guidelines for the diagnosis and treatment of BE12 that recommend not adopting surveillance programs designed in other countries because of controversies regarding high-risk populations. Follow-up is suggested only in patients with intraepithelial neoplasia, according to the Vienna classification13 of the World Health Organization (WHO), but that suggestion is made as an expert recommendation and does not have “hard” epidemiologic evidence to back it up. This reflects the need for recent and robust information on BE in the Mexican population.
The aim of the present study was to determine the frequency and characteristics of BE in patients evaluated at a tertiary care hospital center that had a histopathologic diagnosis of the disease, within a 10-year time frame. The demographic characteristics of the patients (age and sex), the endoscopic findings of BE, presence and type of dysplasia (low-grade, high-grade), and esophageal adenocarcinoma were documented as secondary aims of the study.
Materials and methodsA retrospective and descriptive study on a cohort of patients that underwent upper gastrointestinal endoscopy performed for any indication was conducted. Information was retrieved from the database of the Department of Pathology of the Instituto Nacional de Ciencias Médicas y Nutrición “Salvador Zubirán” (INCMNSZ) within the time frame of January 2002 and December 2012. Patients with a histologic diagnosis of BE were included in the study and those without a histologic diagnosis were excluded.
The endoscopic procedures were performed by staff physicians and residents of the Department of Gastrointestinal Endoscopy after obtaining informed consent. The patients had conscious sedation, cardiovascular monitoring, pulse oximetry, and oxygen through nasal points. Fentanyl, propofol, and/or midazolam were administered at the discretion of the anesthesiologist. Olympus GIF 160, 180, 160z series (Tokyo, Japan) frontal view videoscopes were used. White light was used in all the procedures±vital chromoendoscopy with methylene blue or acetic acid, as well as digital chromoendoscopy with narrow band imaging (Narrow Band Image, NBI, Olympus, Tokyo, Japan) or magnification, as decided by the endoscopist. BE was initially classified as short-segment or long-segment.1 Biopsies were taken based on the Seattle protocol.1 If there was a lesion in a BE segment, it was biopsied. The samples were put in jars of 2% formalin and later processed and examined on hematoxylin and eosin-stained slides by staff physicians from the Department of Pathology. Regarding abnormal epithelium, the pathology studies established whether there was specialized intestinal metaplasia, low-grade dysplasia, high-grade dysplasia, or esophageal adenocarcinoma associated with Barrett's epithelium. At least two pathologists reviewed the biopsies diagnosed with BE and any grade of dysplasia. If the two pathologists did not agree on the grade of dysplasia (low-grade or high-grade), a third pathologist then evaluated the samples. The following variables were analyzed: age, sex, BE length, presence and type of dysplasia at the time of BE diagnosis, and years of follow-up. In addition, the type of medical, endoscopic, or surgical treatment received by the patients with BE was registered.
Definitions- •
BE: the presence of specialized intestinal metaplasia in esophageal biopsies
- •
BE length: length in centimeters; short-segment BE was length under 3cm and long-segment BE was length equal to or above 3cm at the time of diagnosis. Measuring was carried out as follows: the tip of the endoscope was placed at the most distal zone of the BE segment (where the gastric folds begin), observing the centimeters marked in the endoscope at the level of the upper dental arcade (UDA). The endoscope was then withdrawn until its tip was situated at the proximal limit of the BE segment, again viewing the centimeters marked in the endoscope at the UDA. BE length was the difference in centimeters between those two points.
- •
Dysplasia grade: the patients were classified based on the endoscopic study and initial histology report as “without dysplasia” (only specialized intestinal metaplasia) or “with dysplasia” (according to the WHO criteria) and were then divided into low-grade dysplasia and high-grade dysplasia. The presence of esophageal adenocarcinoma was also registered, specifying the type of dysplasia found in the samples of those patients. If dysplasia was undetermined in the initial report, the diagnoses of absence or presence and grade of dysplasia made by the pathologists during the follow-up were then included in the study data.
- •
Years of follow-up: time in years of patient follow-up, from BE diagnosis to the last consultation in the medical records.
- •
Medical treatment: antisecretory treatment with proton pump inhibitor, H2 receptor blocker, or antacid.
- •
Endoscopic treatment: treatment through endoscopic resection of the mucosa, radiofrequency ablation, or both.
- •
Surgical treatment: esophagectomy.
Descriptive statistics were employed, with measures of central tendency (mean and median) and dispersion for a population of parametric distribution (standard deviation) and nonparametric distribution (minimum-maximum interval), according to the variable evaluated. Absolute and relative frequencies were utilized and the differences in the continuous variables between groups were evaluated with the Student's t test or Mann-Whitney U test, as appropriate. The chi-square test or Fisher's exact test were used for the dichotomous variables, in case the expected number of events in a cell was under 5. Statistical significance was set at a p<0.05 and the statistical tests were carried out with the SPSS v.20 (IBM Corp., Armonk, NY, USA) program.
ResultsA total of 43,639 upper gastrointestinal endoscopies were performed. Of those patients, 420 had BE, corresponding to a frequency of 9.6 patients with BE for every 1,000 procedures performed. Of the BE patients, 281 (66.9%) were men and the mean patient age±SD was 57.2±15.3 years. A total of 223 patients (53%) had long-segment BE and 197 (47%) had short-segment BE.
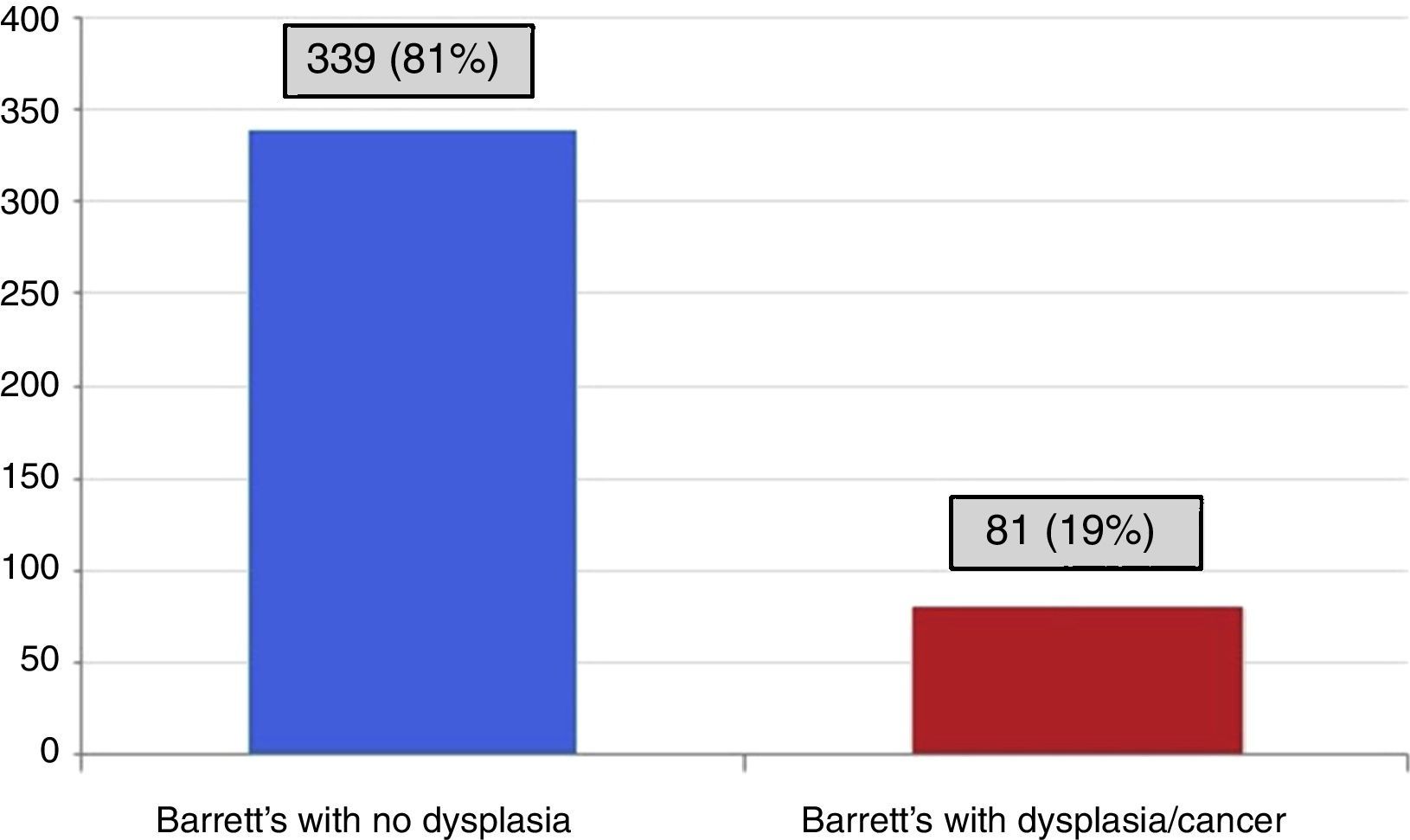
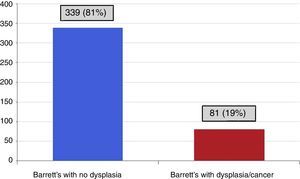
Of the patients evaluated, 339 (81%) did not present with dysplasia and 81 (19%) had some grade of dysplasia or cancer originating in the BE (fig. 1). Of the patients with dysplasia, it was low-grade in 48/81 (58.2%) and high-grade in 20/81 (24.8%) (12 with high-grade dysplasia, alone, and 8 with high-grade dysplasia with esophageal adenocarcinoma). Adenocarcinoma originated in the BE in 13/81 (16.1%) patients.
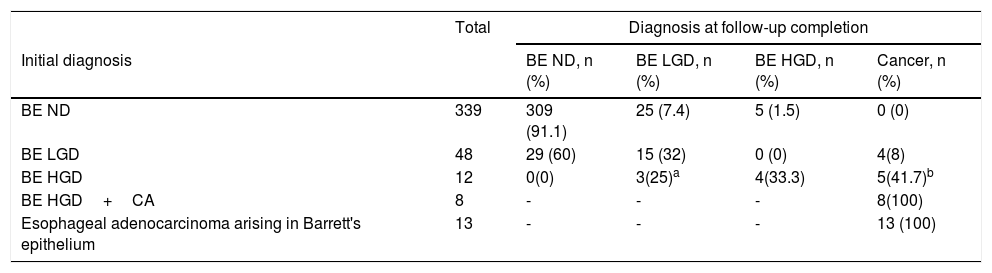
The mean follow-up period was 5.6 years. Of the 339 patients with no dysplasia upon entering the study, 25 (7.4%) progressed to low-grade dysplasia and 5 (1.5%) to high-grade dysplasia. Of the 48 patients with low-grade dysplasia, 15 (31%) remained unchanged, 29 (60%) were reported as BE with no dysplasia, and 4 (8%) progressed to adenocarcinoma. Of the 20 patients with high-grade dysplasia, 8 had coexisting esophageal adenocarcinoma upon entering the study. Of the remaining 12 patients, one progressed to cancer, 4 had no change (3 of whom received endoscopic treatment), and in the other 7 patients, 3 were reported with low-grade dysplasia after mucosectomy and 4 underwent esophagectomy, with a histopathologic report of adenocarcinoma of the esophagus (Table 1).
Follow-up of patients with Barrett's esophagus.
| Total | Diagnosis at follow-up completion | ||||
|---|---|---|---|---|---|
| Initial diagnosis | BE ND, n (%) | BE LGD, n (%) | BE HGD, n (%) | Cancer, n (%) | |
| BE ND | 339 | 309 (91.1) | 25 (7.4) | 5 (1.5) | 0 (0) |
| BE LGD | 48 | 29 (60) | 15 (32) | 0 (0) | 4(8) |
| BE HGD | 12 | 0(0) | 3(25)a | 4(33.3) | 5(41.7)b |
| BE HGD+CA | 8 | - | - | - | 8(100) |
| Esophageal adenocarcinoma arising in Barrett's epithelium | 13 | - | - | - | 13 (100) |
BE HGD: Barrett's esophagus with high-grade dysplasia; BE HGD+CA: Barrett's esophagus with high-grade dysplasia and adenocarcinoma; BE LGD: Barrett's esophagus with low-grade dysplasia; BE ND: Barrett's esophagus with no dysplasia.
According to our results, BE frequency was 9.6 cases for every 1,000 endoscopies performed (0.96% of the upper digestive tract endoscopy total).
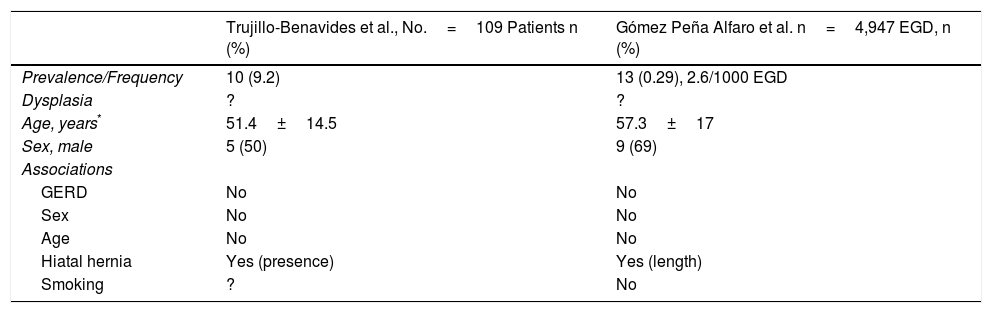
This frequency is lower than that reported in other international case series,3–5 considering that the endoscopies in our study were performed at a single hospital center. Standing out among the most recent reports are a Swedish study3 on 1,000 patients, of which 16 patients (1.6%) had a histologic diagnosis of BE, an Italian study4 on 1,033 patients, of which 13 (1.3%) had a histologic diagnosis of BE, and a Chinese study 5 that included 1,029 patients, 18 (1.8%) of which had a diagnosis of BE, but it was only endoscopic in some of the patients. In relation to data in Mexico, the frequency of BE in the present study (0.96%) was higher than BE frequency reported in a study published in 2005. In that analysis, 4,947 consecutive upper gastrointestinal endoscopies were performed over a 3-year period. A total of 13 BE cases with histologic diagnosis were found, corresponding to a frequency of 2.6 cases for every 1,000 upper gastrointestinal endoscopies carried out (overall frequency of 0.26% of all the studies performed).8 The differences can be explained by the number of endoscopic procedures considered in each study, as well as their time frames. Our data were also different from those of another Mexican study on 109 patients with gastroesophageal reflux disease diagnosed through the Carlsson-Dent questionnaire. They were consecutively referred for endoscopy and 10 cases were diagnosed with BE (prevalence of 9.6%) (Table 2).9 That study was on patients with GERD, whereas ours was on an open population, which can explain the differences in frequency. Patient age in our study was similar to that of other case series, as was predominance in the male sex.3–5 The majority of our study patients had long-segment BE (53%), differing from other studies in which short-segment BE predominated.9–11 This could be due to the fact that the INCMNSZ is a referral center. The number of patients with dysplasia were in the minority and they were subdivided from greater to lower frequency into low-grade dysplasia, high-grade dysplasia, and esophageal adenocarcinoma arising in Barrett's epithelium. These data were similar to those in the majority of the international case series.3–5 Progression over time was stable in the majority of our sample and changed only in a minority of patients. Upon analyzing the initial 48 patients with BE and low-grade dysplasia, 15 (31%) had no changes, 29 (60%) were later reported to have BE with no dysplasia, and 4 (8%) were reported to have adenocarcinoma. This can be explained by the sampling variations for obtaining the tissue during the endoscopy or by the differences in the analysis and interpretation of the biopsies, situations that have been reported in previous studies.14,15 In the present case series, we observed that BE with high-grade dysplasia tended to progress to adenocarcinoma with greater frequency, compared with the BE in patients with no dysplasia or with low-grade dysplasia. Therefore, we believe that patients with high-grade dysplasia should undergo endoscopic and/or surgical treatment in accordance with the experience of each hospital center or be referred to centers specializing in the integrated evaluation of patients with BE.
Data and demographic characteristics in the Mexican populations of previous studies8,9
| Trujillo-Benavides et al., No.=109 Patients n (%) | Gómez Peña Alfaro et al. n=4,947 EGD, n (%) | |
|---|---|---|
| Prevalence/Frequency | 10 (9.2) | 13 (0.29), 2.6/1000 EGD |
| Dysplasia | ? | ? |
| Age, years* | 51.4±14.5 | 57.3±17 |
| Sex, male | 5 (50) | 9 (69) |
| Associations | ||
| GERD | No | No |
| Sex | No | No |
| Age | No | No |
| Hiatal hernia | Yes (presence) | Yes (length) |
| Smoking | ? | No |
The limitations of the present study were that it was a retrospective study conducted at a tertiary care hospital center, which can result in reference bias. However, ours is the study with the largest number of histologically diagnosed patients with BE in Mexico that specified the presence and grade of dysplasia, as well as the follow-up over time.
In conclusion, according to the present study the frequency of BE in a sample of Mexican patients was 9.6 cases per every 1,000 upper gastrointestinal endoscopies. Dysplasia was not reported in most of the patients with BE and the majority had no histopathologic changes in the follow-up period. A total of 19.3% of the patients presented with dysplasia or cancer.
Ethical disclosuresProtection of human and animal subjectsThe authors declare that no experiments were performed on humans or animals for this study.
Confidentiality of dataThe authors declare that no patient data appear in this article.
Right to privacy and informed consentThe authors declare that no patient data appear in this article.
Conflict of interestThe authors declare that there is no conflict of interest.
Please cite this article as: Valdovinos-Andraca F, Bernal-Méndez AR, Barreto-Zúñiga R, et al. Esófago de Barrett: experiencia de 10 años en un centro de tercer nivel en México. Revista de Gastroenterología de México. 2018;83:25–30.